Athlete’s Foot
Athlete’s foot is a common skin infection found in a group of related fungal skin infections known as tinea. The medical terms associated with athlete’s foot include tinea pedia, plantaris, dermatophytosis Palmaris, and interdigitalis. These infections are caused by a number of mold-like fungi, known as dermatophytes, which reside in dead tissues on the hair, skin and nails.
Only those who have experienced athlete’s foot first hand know how uncomfortable the infection can be. Athlete’s foot typically occurs on the soles of the feet but can spread to areas between the toes and the toenails. The condition can also be spread by contact such as touching your foot then touching other areas of the body including your hands, palms, underarms or groin.
Symptoms
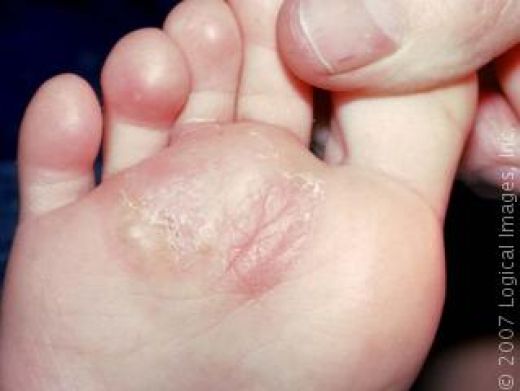
Symptoms of athlete’s foot can vary depending on the individual, stage and severity of the infection, and how the body reacts.
Some individuals experience an allergic reaction to the fungus that causes athlete’s foot.
Athletes Foot? Get Remedies Fast!
This is called an ‘id reaction’ and can result in vesicles or blisters on areas of the body like the arms, hands and chest.
Treatment of the id reaction is usually cured with treatment of athlete’s foot.
While other symptoms may be present in individuals experiencing athlete’s foot, here you will find a list of the most common symptoms associated with the infection.
Symptoms Include
- Peeling and cracking of the skin around and between the toes
- Intense itching on the soles of the feet and surrounding area
- Redness or inflammation that worsens as the infection progresses
- Blisters on the soles of the feet as well as along the sides of the feet
- Scaling and flaking on the soles of the feet and in between the toes
- Burning or stinging sensation in the area of the infection
- Crusting or oozing of the soles of the feet that may spread to the toes
- Thick, discolored and crumbled skin if the fungus spreads to the nails
- Any of the above symptoms can also occur on other body parts if spread
Causes
Athlete’s foot is caused by dermatophytes, tiny parasites that live on certain areas of the body including the skin. Dermatophytes can be divided into three separate groups according to which host they prefer.
- Zoophile – Fungi that prefers an animal host
- Geophile – Fungi that prefers a soil host
- Anthropophile – Fungi that prefers a human host
In the majority of cases, athlete’s foot is caused by the anthropophile fungi as it favors a human host. The three most common species of anthropophile fungi include Epidermophyton, Microsporum, and Trichophyton. These three species account for more than 90 percent of all fungal infections that occur on the skin.
Athlete’s foot is not limited to only athletes or those who are in good physical shape. The infection can occur on any person that remains damp or moist on their foot or feet for a certain period of time. Those who wear tight fitting clothing or those who don’t dry their feet properly on a consistent basis are more at risk for athlete’s foot.
Every person is acceptable to athlete’s foot as we all have one or more of the fungi in our bodies. Most of these fungi are harmless and simply feed on dead skin cells. Athlete’s foot is more common in young individuals and adults. The condition is also highly contagious and can be spread on our own bodies or to others. This can occur through skin-to-skin contact or indirectly through objects such as shoes, floors, towels, clothing, etc.
Risk Factors
Certain individuals are more at risk for developing athlete’s foot depending on certain lifestyle conditions and choices. Clothing options such as closed toe shoes (especially plastic lined shoes) and thick socks that cause sweating of the feet for a long period of time can lead to the infection.
Those who sweat profusely while working, exercising or participating in other daily activities are also at risk.
Although you may not experience any of the above factors, you may still be at risk if you work, study or play in a public area. Direct contact with an infected person or with materials that are infected with the parasites such as socks, shoes, public showers or gyms can cause the spread of athlete’s foot to an area on your own body. The risk is greater when the environment is warmer as this is grounds for the fungus to grow and invade the skin.
Risk Factors Include:
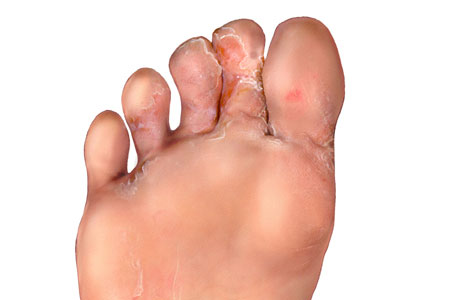
- Not keeping your feet dry, clean and maintained
- Excessive perspiration
- Humid, warm or hot weather or environment
- Disorders or conditions of the immune system
- Prior infections of athlete’s foot
- Wearing tight, close toed shoes or poorly ventilated shoes
- Walking barefoot at home or in public areas
Prevention Tips
Treatment of athlete’s foot begins with preventing the infection from occurring in the first place. For those who are prone to athlete’s foot, prevention is a much bigger issue that can be maintained through a variety of effective tips and techniques.
Since athlete’s foot can easily be spread from person to person, it’s important to keep your family and community safe by not sharing or leaving infected items where others could potentially come in contact with the materials.
Keep places where your feet touch such as floors, showers, bathtubs, and beds clean and maintained. When in public areas such as swimming pools or gyms, keep a pair of flip flops handy to prevent walking on the floor and picking up or spreading the infection. Disinfectant spray should be used in kitchens and bathrooms in the home. Clothing, towels, bed sheets and blankets should be washed on a regular basis in hot water to help kill the growing fungus. Be sure not to leave moist or damp dirty laundry lingering in the washer or hamper for any period of time to avoid the spread of parasites. Avoid sharing these types of materials among family members and consider doing separate loads of wash.
Special soaps can be used on a regular basis to prevent fungal infections such as athlete’s foot. These fungal soaps contain active ingredients, such as tea tree oil, that help fight off and prevent the infection. They also contain Aloe Vera and are free of chlorine and sediments, leaving your skin moisturized and smooth.
Consider sanitizing the inside of your shoes with a germicidal shoe tree. This will help keep your shoes free of fungal parasites. Keep your feet dry by applying an antiperspirant made especially for feet perspiration. Replace the inserts of your shoes on a regular basis and replace any old exercise shoes or sneakers. After participating in any type of physical activity, use a soap that contains anti-fungal agents and antibacterial qualities. Try to wear open toed shoes or sandals whenever possible to allow your feet time to breathe and receive fresh air.
Test and Diagnosis Considerations
Typically, the diagnosis of athlete’s feet is made by a general doctor or podiatrist (foot doctor) by a visual exam of the foot or feet. Skin scrapings may be needed to test for the specific type of fungi the patient is experiencing to determine the best route of treatment. Microscopic examinations may also be needed to rule out more serious problems such as a bacterial infection.
Various tests may be recommended, such as a fungal culture or an examination of the patients’ foot under ultraviolet light. Your doctor may also do a potassium hydroxide (KOH) test to diagnosis athlete’s foot. This is done by carefully scraping scaly skin from the soles of the feet and placing them onto a microscope slide. KOH is then added to the slide and it’s placed beneath a microscope to look for signs of fungus. In many cases, a doctor will be able to diagnosis athlete’s foot simply by sight.
Common Symptoms
It’s important to rule out other causes of common symptoms associated with athlete’s foot. Peeling or redness of the feet may be caused by environmental factors such as tight shoes, excessive perspiration due to warm weather or wearing shoes without socks. Adhesive cements and certain dyes found in some types of shoes can also cause irritation to the feet.
Other similarities to the symptoms of athlete’s foot can be due to nail polishes, lotions or powders that the patient applied their selves that caused irritation. Conditions such as scabies, eczema and psoriasis may be other possibilities for your symptoms. It’s best to talk to a doctor to rule these out.
If all attempts for diagnosis of athlete’s foot come back inconclusive, a biopsy of the infected skin can be taken for examination. Your doctor may recommend you to a special physician, such as a dermatologist (skin doctor), podiatrist (foot doctor) or a foot health practitioner to future examine your condition. Once a proper diagnoses is made, your doctor can recommend effective treatment methods for you to consider and may write you’re a prescription for a topical or oral medication to help treat the infection.
Treatment Options
There are many over the counter, natural and home remedies available for the treatment of athlete’s foot. While some of these treatments are highly effective in curing the infection, others simply treat the symptoms causing reoccurring episodes. Not everyone responds to all treatments so it’s best to talk to your doctor to see which may be the best fit for you. This could depend on your allergies, medical history, current conditions and various other factors.
Herbal & Home Remedies: Herbal treatments are popular as they are usually effective in treating the condition and have little or no side effects. Common herbal and home remedy treatments for athlete’s foot include tea tree oil, Listerine (mouth wash) and hydrogen peroxide. To sooth and treat your sore feet, soak them in a solution of two teaspoons of salt per one pint of warm water. These home remedy provides an unappealing environment for fungus and makes over the counter treatments more effective. A solution of 25 percent aluminum chloride and water provides similar results.
Fungus Between Your Toes
For fungus between your toes, a mixture of baking soda and water can be used to form a paste. Rub the paste onto the site of the infection, allow drying time then rinse with warm water. While in the shower, use a foot brush to rub away dead skin cells, leaving smooth new infection free skin. Remember to continue applying a foot cream or powder, wearing dry socks and choosing shoes that fit well and allow your feet to breathe.
Alternative treatments may also be used to treat athlete’s foot. The following oils and extracts have been found effective in relieving symptoms of athlete’s foot and with regular use, treating the infection: Topical oils (example-tea tree oil), onion extract, garlic extract, boric acid and Epson salts. Rubbing one or more of the following products on your feet twice a day or in a mixture of warm water can lead to foot relief.
Herbal & Home Remedies Include
- Keep feet as dry as possible, especially between the toes
- Wear cotton socks and change them once or twice per day
- Avoid tight closed toed shoes as these cause heat build-up
- Never go in public areas barefoot, especially moist or warm areas
- Apply foot creams and powders regularly to keep feet healthy
- Always wash your socks in hot water to kill all potential bacteria
- Avoid yeast products such as baked goods and breads
- Vinegar and alcohol should not be consumed by chronic sufferers
- Apply grapefruit seed extract to your feet to fight off fungus
Pharmaceutical Remedies
Over the counter and prescription athlete foot creams, powders and liquids are available. These usually contain active ingredients such as clotrimazole, miconazole and tolnaftate. If used on a regular basis, these types of treatments usually work well but may take longer to see results. Athlete foot powders work by keeping the feet dry throughout strenuous activity and perspiration.
Along with these self-care tips, keeping your feet dry and clean, washing your feet frequently with warm soap and water and wearing dry, clean socks can help keep the infection under control. If the over-the-counter remedies fail to work after two to four weeks of use, you may want to consider visiting your doctor for a stronger medication. Your doctor may prescribe a topical or oral medication such as terbinafine or ketoconazole to treat the fungus. Antibiotics may also be needed for bacterial infections.
Side effects from oral athlete’s foot medications may include rashes, gastrointestinal upset and abnormal liver function. The Food and Drug Administration (FDA) issued a warning against oral Lamisil and Sporanox in May of 2001 due to links between the medication and rare cases of liver failure and even death. They also have a history of weakening the heart contractions so they should be avoided by those with heart problems.

1 Comment
Hi ,
may i know can i get the pic of the athlete foot in high res? or whr can you can the pic?
Are you allow me to use as commercial usage?
Thank you!