Many new mothers agree that breastfeeding is one of the great pleasures of having a newborn. It can be a healthy, bonding experience, both physically and emotionally, for both mother and baby. Unfortunately, sometimes infections can occur that make breastfeeding very painful.
Mastitis is an inflammation of the breast caused by bacteria. Unlike engorgement or a plugged duct, mastitis normally requires an antibiotic. It occurs most often in women who are nursing. This is called lactation mastitis. It occasionally happens in women who are not nursing or pregnant.

Symptoms
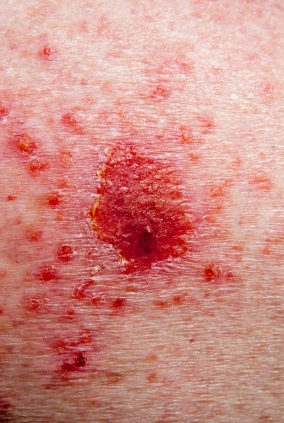
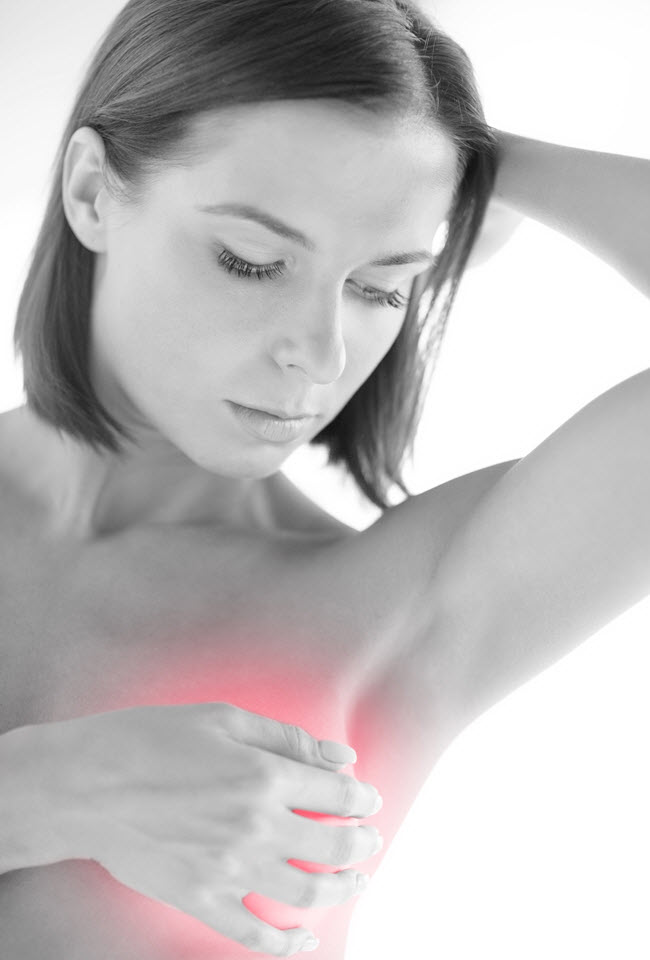
Mastitis can cause pain, swelling, redness, fatigue, high fever, flu-like symptoms and chills. There may be a tender lump and the area may be hot to the touch and swollen. There may be a burning sensation in the breast.
The lymph nodes under the armpit or above the collar bone may also be sore and swollen. In severe cases, there may be pus draining from the nipple. Lactation mastitis normally affects only one breast.
Flu-like symptoms are usually the first sign of mastitis. A sore red area may appear on the breast a few hours later. A call to the doctor should be made at this point to determine whether or not an antibiotic is needed.
Causes
Approximately one nursing mother out of twenty will get a breast infection. Bacteria can pass from the baby’s nose, mouth and throat through a crack or sore in the mother’s nipples. The bacteria can then infect the milk ducts and glands. Mastitis can also develop in the breast without broken skin, but it is not as common. Mastitis can happen at any point in a mother’s nursing career, but within the first month is the most common. Some tips on the causes of Mastitis are:
- A mother that is run down will be more susceptible to infection. It is important for a mother who is breast feeding to eat a healthy, well balanced diet and to take naps when possible. The demands of a new born can be very tiring.
- Once a woman has developed mastitis in the breast, it is more common to have a recurrence. If a mother continually misses feedings or gives a bottle in place of a feeding without pumping, the chances of another episode is increased.
- Not fully draining the breast, or nursing in only one position, may increase the chance of mastitis. Milk stasis can occur if there is milk left in the breast. Milk that sits in the breast has an easier chance of becoming infected.
- Wearing a bra that is too tight or confining can restrict milk flow, which increases the chance of infection.
- Allowing the breasts to become engorged can cause the ducts to clog and become infected.
- Poor attachment to the breast can cause an increased chance of mastitis. Normally, when the baby isn’t latched on well, all of the milk can’t get drained from the breast.
Conventional Treatment
A physical examination and the patient’s medical history will be the determining factor of whether or not an antibiotic is needed. It is not always easy to tell the difference between plugged ducts, engorgement or infection. If a plugged duct or engorgement is the cause of pain, it will gradually begin to feel better without medication. If mastitis is the cause of pain, the mother will continually feel worse.
Oral antibiotics are usually given to fight a mastitis infection. The antibiotics are usually successful for treatment as long as the full prescription is taken. The most common brand name antibiotics are biocef, keflex, keftab and pathocil. Side effects of the penicillin-based antibiotics are rare. If they do occur they are mild.
Some of these can include nausea or vomiting, intestinal gas, loose stools or diarrhea and skin rashes or itching. The side effects of the cephalosporin drugs are also rare, but may include mild forms of diarrhea, abdominal pain, skin rashes or itching and vaginal yeast infections. A small amount of the antibiotic taken will enter the breast milk, but this will not harm the baby.
Getting Treatment Quickly
When mastitis isn’t properly treated or treated too slowly, abscess may develop. A collection of pus can develop in the breast. This usually requires surgical drainage, which often requires a general anesthesia. A breast surgeon may have to use a needle guided by an ultrasound scan to drain the abscess.
Ice, Heat, and Rest
Alternating warm and cold compresses on the inflamed area can help to relieve the pain. Heat to the breast can help increase circulation and milk flow. This may help fight the infection and get things moving. Also, massaging the area that is tender may help to loosen the ducts that have become plugged.
Getting lots of rest and drinking plenty of fluids while the breast is infected is important. Ten to twelve glasses of water should e consumed per day. This will help keep the milk supply flowing and the body functioning to fight infection. A mother should treat herself just as she would when she has a virus or flu.
Some additional treatment tips include:
- Keep the inflamed breast emptied by nursing frequently or by pumping the breast. Nurse every two hours on the affected side, if possible.
- Taking ibuprofen will help relieve some of the pain and discomfort of mastitis.
- After taking antibiotics for 24-48 hours, the pain will start to subside and the mother will begin feeling better.
Natural Remedies
There are some different alternatives to curing matisis besides giving a woman antibiotics. Because some of the antibiotics can be given to the baby through nursing, some women would rather take a holistic approach. These are some of the things women who don’t want antibiotics are trying:
Use frozen, raw cabbage leaves. They can reduce pain and inflammation. They help draw out the heat and infection. Place the leaves directly on the infected area. The cabbage leaves should be replaced when they reach room temperature (there is controversy with this method from some conventional method doctors).
Additional Natural Remedy Options
Make a poultice of comfrey leaves and calendula flowers. Apply hot applications to the infected breast four times daily. This will soothe the nipples and help draw out the infection.
Other natural remedy options are to use one dropper full of Echinacia root tincture, six times a day while the infection is bad and then reduce to 2 or 3 times a day and oriental medicine experts think that acupuncture can help clear the toxic heat and treat underlying imbalance that may be causing the mastitis.
Plants & Herbs for Treating Mastitis
A variety of plants and herbs are thought to help with the healing of a breast infection:
- Echinacea root – known as an antibiotic alternative that helps to fight infection.
- Prickly ash – increases the immune system and stimulates the lymphatic flow. It helps dissolve
- blockages.
- Cleavers – helps to reduce swelling.
- Calendula – promotes the flow and drainage of lymphatic fluid. It helps dissolve blockages.
- Hytolacca – used for sensitive cracked nipples and blocked milk ducts.
- Pulsatilla – used for sore nipples and to help lift a mother’s mood.
- Belladonna – used for inflamed breasts that have red streaks radiating from the nipples, heat
- and throbbing pain.
- Bryonia – used for heavy, hard and painful breasts.
- Silica – used for cracked and infected nipples.
Prevention

Wear loose fitting clothing that does not irritate or rub the nipples. Don’t wear tight fitting or constricting tops. Wearing a properly fitting nursing bra will also help. A nursing mother should keep her nipples clean and dry between feedings. This will help reduce the risk of infection
Make sure the baby is attached properly to the breast. The baby has to latch on correctly in order to obtain an adequate amount of milk. There must be a tight seal around the nipple and most of the areola.
Changing the baby’s position will help to ensure that each breast is completely drained of milk each feeding. Milk stasis can occur if there is milk left in the breast. This can cause excess pressure and milk may leak into breast tissue, which can cause inflammation.
Avoiding Engorging
When a mother’s breasts become full, she should have her baby nurse to make sure she doesn’t get engorged. If she does become engorged, the breast needs to be promptly relieved. A mother should wake her baby every four hours to nurse in the early weeks of birth. She may have to remove blankets, change the baby’s diaper or massage her baby’s back, arms and legs to get the baby awake enough to nurse.
A baby should be weaned gradually to prevent engorgement and inflammation. Many mothers will start out by cutting one nursing session every three or four days. Drop the least favorite feedings first. The morning and evening feedings will usually be the last to go. This process will likely take two or more weeks.
The slower the process, the more likely the breasts will be protected from engorgement and infection. Also, weaning slowly will help the baby to have less anxiety.
Sleeping Tips
A nursing mother should get plenty of rest and eat a healthy, well-balanced diet. She may become more susceptible to infection because of the lack of sleep and stress of having a newborn. Avoid sleeping on your stomach. It can restrict the flow of milk in the breast.
Nursing
Normally, a mother is still able to nurse her baby when she is diagnosed with mastitis, although it may be very painful. It is important that the infected breast stays drained. If the baby won’t nurse on the infected side, it is important to pump the breast until it is emptied of all milk. The milk may taste a little different with the infection, but most babies don’t seem to mind.
Because of the pain associated with mastitis or other breast infections, some mothers may feel they should give up breast feeding their babies. The pain and problems that they have to endure are just too much to handle. However, there are many benefits to the mother and her baby when nursing is chosen.
Why Use Breast Milk?
Breast milk is easier for a baby to digest than formula. It is rich in nutrients and antibodies that will help protect the baby from germs and illness. The mother and baby tend to bond better when nursing is the choice. They may feel more warm and secure due to the close physical contact.
The surgeon general reports state that breast milk is the best source of nutrition for infants. Breastfeeding has been shown to protect babies against otitis media, gastroenteritis, severe lower respiratory infections, and necrotizing enterocolitis. It has also been associated with lower rates of sudden infant death syndrome, childhood obesity, type 2 diabetes, and leukemia.
A mother’s health benefits include a reduced risk for type 2 diabetes, as well as breast and ovarian cancers. It has also been shown to help with postpartum depression.
Breast Milk Saves Money
Not having the cost of formula or the hastle of sterilizing bottles and nipples, along with the optimal nutrition and health benefits for mother and baby, make nursing an easier choice .



 If this test points toward a case of lactose intolerance, a follow up blood test can be done to confirm the lack of broken down sugars in the bloodstream. For babies and small children who cannot be exposed to the high level of lactose required for testing, a stool sample can be analyzed for excess amounts of lactic acid that has passed through the colon.
If this test points toward a case of lactose intolerance, a follow up blood test can be done to confirm the lack of broken down sugars in the bloodstream. For babies and small children who cannot be exposed to the high level of lactose required for testing, a stool sample can be analyzed for excess amounts of lactic acid that has passed through the colon.