Frequent Urination Condition
Frequent urination simply means urinating more often than usual. Its a symptom rather than a condition. Most people empty their bladders between four and eight times a day; frequent urination is therefore defined as voiding urine more often than eight times a day with the implication that this increased rate is not strictly volitional.
Frequent urination does not always signify an underlying health problem.
You may be drinking too much fluid, or possibly you need to modify your food and beverage intake: alcohol, caffeinated beverages such as coffee and tea and even some foods such as celery, watermelon and parsley are natural diuretics increasing the amount of urine you would normally excrete.
Underlying Problems
But frequent urination is often a sign of an underlying medical pathology, most often a urinary tract infection or cystitis (an inflammation of the bladder) that can affect either sex although it most common in women.
Frequent Urination? Get Remedies Fast!
Frequent urination can also be the first symptom of diabetes, both type 1 and type 2, as the body mobilizes the urinary system to rid itself of excess glucose.
Frequent urination is linked to prostate problems in men and to pregnancy and pelvic inflammatory disease in women. The symptom is also a common side effect of obesity and abdominal radiation treatments.
Even when frequent urination is not connected to an underlying pathology, it can be a disruptive and embarrassing condition. When you have to go, you have to go no matter what else is happening around you.
When frequent urination forces major changes in lifestyle habits or is accompanied by fever, pain, nausea and vomiting, increased or decreased appetite, genital discharge or changes in the appearance of the urine itself, it’s time to consult a physician about the condition.
Alternative Names
There are several different conditions which are closely associated with frequent urination:
Urgent Urination, Urinary Urgency
A sudden, compelling need to urinate linked to a burning sensation or pain, often a sign of an underlying urinary tract infection.
Urge Incontinence, Urinary Incontinence, Overactive Bladder Syndrome
A sudden, irresistible need to urinate due to bladder spasms. Symptoms include urinary frequency, urinary urgency, and sometimes leaking urine before you can get to a toilet.
Stress Incontinence
Involuntary urination that occurs during an activity such as coughing, sneezing or laughing, generally caused by an underlying anatomic weakness to the bladder.
Nocturia
Frequent urination at night involving waking up several times to use the toilet.
Polyuria
The production of excessive volumes of urine for an adult, over 2.5 liters in 24 hours.
Depending on the underlying cause of your urinary frequency, you may experience some of these symptoms as well.
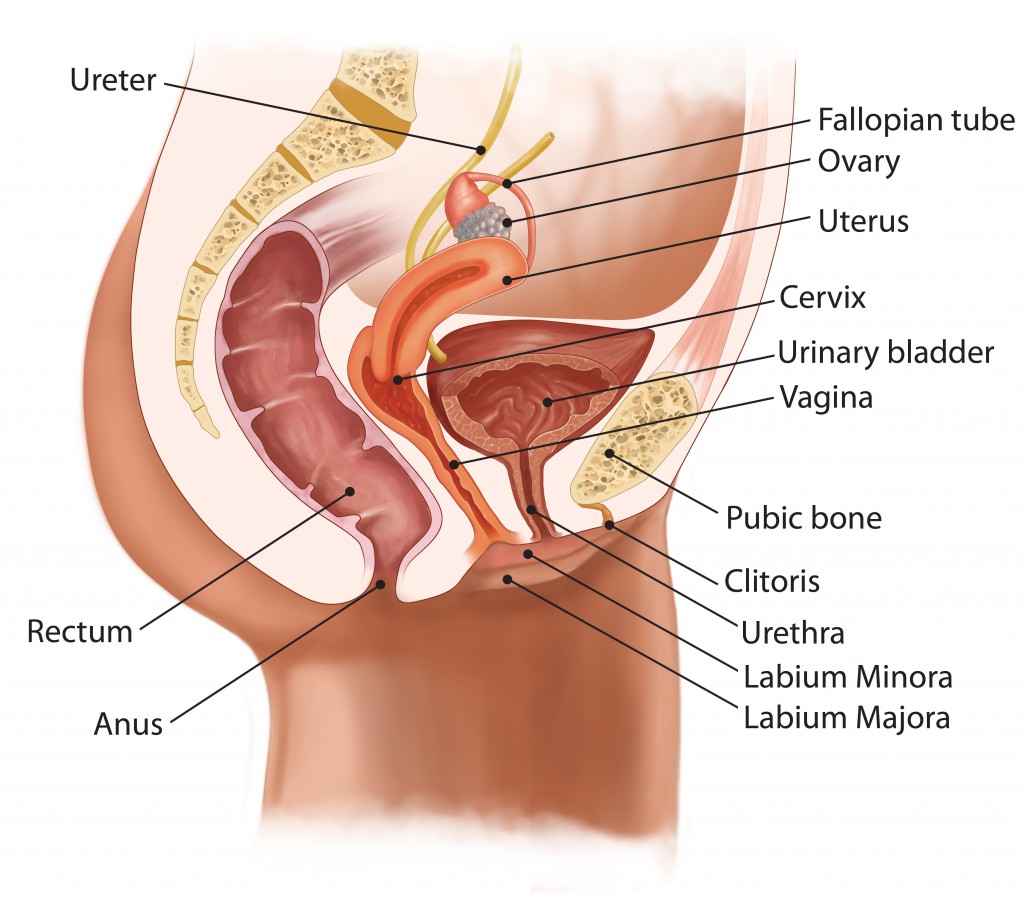
Physiology
Urination is the process by which urine is eliminated from the body, a function which in healthy humans is partly under voluntary control.
Cellular metabolism generates nitrogenous waste products that must be eliminated from the bloodstream. These wastes are filtered out of the bloodstream by the kidneys. There are two kidneys in the body, each made up of microscopic structures called nephrons that act as filtering units removing most of the water, salt and waste from the blood that passes through them.
The resulting liquid waste product called urine is transported through anatomic structures called ureters to the bladder where it is stored. The anatomical structure of the ureters and bladder do not allow urine to back up towards the kidneys under most circumstances.
Bladder Muscles
The bladder has two sets of muscles controlling its opening. Only the external sphincter is under voluntary control. Both the internal sphincter and the smooth muscle in the wall of the bladder are under the control of the parasympathetic nervous system. As your bladder fills with urine, the smooth muscle stretches by means of small contractile waves to accommodate the extra volume of urine. When urination occurs, the bladder’s outer layer of muscle (called the detrusor) contracts to help push out urine.
Urine is excreted from the bladder through the urethra, a process called urination. The average adult bladder can hold between 300 and 500 cc of urine. Urine is sterile when it is excreted from the body: it contains fluid, salts and waste products, but it is free of bacteria, viruses and other pathogenic organisms.
Causes of Frequent Urination
Overactive Bladder
Overactive bladder is a condition associated with a sudden, irresistible urge to urinate, resulting from involuntary contractions of the musculature of the bladder wall.
Overactive bladder is particularly common among middle-aged and older adults, and some medical experts estimate that one out of ever 11 adults in the United States suffers from some form of it. Untreated overactive bladder can lead to an increased incidence of urinary tract infections and skin infections from the corrosive effects of urine on the delicate skin of the urogenital area. But treatment success rates are high: with behavioral modification techniques and medication, 80% of people are able to bring their symptoms under control.
Overactive bladder can be brought on by abnormalities of the nervous system such as spinal cord injuries, multiple sclerosis, strokes, Parkinson’s disease and diabetic neuropathy; by urinary tract infections; and by blockages to the urinary system such as those caused by kidney stones or an enlarged prostate. But in many cases, there is no underlying pathogenic cause to overactive bladder.
Medical History
Medical history plays an important role in diagnosis: urinary frequency, urinary urgency, stress incontinence and urinating more than three times a night are all suggestive of overactive bladder. A pelvic exam for women (to rule out pelvic inflammatory disease) and a prostate exam for men (to check for enlargement) are generally indicated. Ultrasonic measurement of the post-void residual (the amount of urine left in the bladder after urination) can further help determine whether symptoms are due to muscle spasms or some other cause.
If underlying pathology is ruled out then treatment for overactive bladder focuses on:
Improving the Tone of the Surrounding Pelvic Muscles
Doing Kegel exercises (also called pelvic floor exercises) for five minutes, two to three times a day, can markedly decrease incontinence in both women and men. Occasionally Kegel exercises are used in conjunction with biofeedback and electrical stimulation of the floor of the pelvis.
Behavioral Modification
Behavioral techniques called bladder training can teach you to resist the urge to urinate, gradually increasing the interval between trips to the toilet.
Medications
Several medications that block the effects of the neurotransmitter acetylcholine have proven successful in the treatment of overactive bladder. They share common side effects including dry mouth, constipation, blurred vision, and in the elderly, confusion.
- Oxybutynin (Ditropan): Oxybutynin suppresses spasms in the smooth muscles of the bladder wall. Additionally it relaxes the detrusor.
- Tolterodine (Detrol, Detrol LA): Tolterodine suppresses spasms in the smooth muscles of the bladder wall. It does not cause the mouth to dry out as much as Oxybutynin.
- Solifenacin (VESIcare). Similar to Tolterodine, but with a longer half-life.
- Tricyclic antidepressants such as imipramine (Tofranil) and doxepin (Sinequan, Adapin) have also been used to treat overactive bladder with some success. Their mechanism of action is not clear.
Natural Treatments
If you are suffering from the symptoms of overactive bladder, there are a number of remedies you can try at home without seeking medical attention. Regulate your fluid intake. If you smoke, stop. Consider eliminating coffee, tea and other caffeinated beverages and foods: caffeine is a known diuretic.

Foods such as chocolate, spicy cuisines, alcohol and carbonated drinks can also irritate the bladder. If you are even a few pounds overweight, consider going on a diet: middle-aged people tend to put on weight in their abdomen, and all that extra avoirdupois exerts extra pressure on your bladder.
Constipation, similarly, also exerts extra pressure on your bladder so consider increasing the amount of fiber in your diet if you suffer from it.
Some naturopathic doctors believe that overactive bladder is linked to food sensitivities, particularly to wheat and dairy products.
These foods, it’s speculated, cause a systemic inflammation that manifests, among other things, as an inflamed bladder. By cutting out one food group for a period of time and observing how your symptoms respond, you can pinpoint the dietary culprit.
Mineral Supplements
A number of botanicals and mineral supplements have also been used to treat overactive bladder with some success.
Pumpkin
Native Americans have used pumpkin seeds for centuries to improve bladder and prostate health. Pumpkin is also one of the few natural remedies to be tested in clinical trials: in one six-week study of postmenopausal women suffering from overactive bladder, almost 60% of participants showed marked improvement.
Magnesium
Clinical trials have also proven the efficacy of magnesium, particularly among patients suffering from Parkinson’s disease. It thought to control smooth muscle spasms.
Saw Palmetto
Palmetto is commonly used throughout Europe to treat the symptoms of benign enlarged prostate. Its precise mechanism of action is unclear but it has anti-inflammatory properties and is known to reduce the activity of enzymes linked to prostate problems. Clinical studies have proved that it reduces urinary frequency. But palmetto has some mild estrogenic effects; for that reason, women who are pregnant, breastfeeding, taking birth control pills or undergoing hormone therapy should avoid it.
Stress Incontinence
Stress incontinence is the involuntary loss of urine due to a sudden pressure on the abdominal muscles secondary to physical activities like coughing, sneezing or laughing.
While its symptoms and many non-invasive treatments are similar to those for overactive bladder, its underlying cause is quite different: it due to a weakening of the pelvic musculature which in men can occur following a prostatectomy and among women is a common aftermath to childbirth among women (exacerbated when estrogen levels decrease in the week before menstruation or following menopause.)
In addition to the treatments described under overactive bladder above, one non-surgical treatment that sometimes used for women suffering from stress incontinence is the insertion of a small ring-shaped medical device called a pessary into the vagina. The pessary reduces stress incontinence by compressing the urethra against the symphysis pubis bone. If a woman uses this treatment option, she must be carefully monitored by her physician to reduce the chance of contracting a vaginal or urinary tract infection.
Surgical treatment is only considered if other non-invasive treatments have failed and the exact anatomical site of the pelvic muscle weakness is known.
Nocturia
Nocturia is the medical term for frequent urination at night. It can be a symptomatic of a systemic disease process such as a kidney or bladder infection, diabetes or sleep apnea; in men, it is often the first sign of prostate enlargement. But even when its causes are relatively benign, nocturia can still be a difficult condition to live with because it interferes with sleep.
Interventions to try at home include minimizing all fluid intake but particularly caffeine and alcohol for at least three hours before bedtime, taking medications that have a diuretic effect earlier in the day, and avoiding strenuous exercise and potentially stressful interactions before sleep. You should see your physician if nighttime urination is accompanied by fever, pain or discomfort, or if your urinary frequency is not affected at all when you cut down on fluids before bedtime.
Medical History and Testing
Since nocturia is frequently a symptom of an underlying systemic pathology, when you visit your physician, he or she will try to rule these out by taking a thorough patient history, performing a physical exam, and ordering diagnostic tests such as urinalysis, urine culture, blood sugar and BUN/creatinine clearance.
Nocturia can be a symptom of benign prostate enlargement, urinary tract infection, kidney failure, congestive heart failure, obstructive sleep apnea or diabetes.
Urinary Tract Infections (UTI)
Urinary tract infections are the second most common type of infection, resulting in 8.3 million visits to doctors offices every year. UTIs are named differently according to the primary site of infection:
- Urethritis is an infection of the urethra
- Cystitis is an infection of the bladder
- Pyelonephritis is a kidney infection
In addition to urinary symptoms like urinary frequency and urinary urgency, UTI symptoms can include low-grade fever, abdominal or back pain, and urine that appears cloudy and has an unusual or foul odor. With more serious infections that spread to the kidneys, symptoms may include a fever over 101 degrees Fahrenheit with chills and night sweats, nausea and vomiting and more severe pain in the abdomen or lower back or referred to the flank.
In a significant number of cases, UTIs are asymptomatic. Indeed among the elderly for whom UTIs are a huge concern, the only symptoms may be confusion, combativeness or other changes in mentation.
UTIs occur when bacteria contaminate the urethra opening and begin to multiply. The most common contaminant is Escherichia coli (E. coli), a bacteria which typically lives in the intestines and the most common source of infection in active individuals is fecal contamination following bowel movements. But any abnormality in the urinary tract that obstructs the free flow of urine a kidney stone, for example, or an external catheter can set the stage for infection.
Higher Risk Categories
Women are more prone to UTIs than men, possibly because their urethras are shorter and closer to the anus. Medical experts estimate that half of all women will experience a UTI at least once in their lifetime, and most of them more than once. Factors that increase a woman™s susceptibility to UTIs include sexual activity (because intercourse can irritate the urethra,) use of the diaphragm as a birth control device, and aging since the decrease in estrogen following menopause leads to more fragile urogenital tissues.
If the UTI involves mild discomfort but no fever, you can try to manage it at home. Your goal will be to flush the offending microorganisms by drinking lots and lots of water. Avoid drinking caffeinated beverages such as coffee and tea, alcohol and carbonated beverages as these will irritate your bladder. Since an ounce of prevention is worth a pound of cure, for the future remember to wipe from front to back after a bowel movement (rather than the other way around), to urinate as soon as possible after sexual intercourse and (for women) to avoid potentially irritating feminine hygiene products.
Cranberry Juice
For more than a century, cranberry juice has been used as a natural remedy for UTIs. Cranberries contain substances called proanthocyanins which seem to prevent bacteria from sticking to the walls of the urinary tract. Don’t use the highly sweetened cranberry juice you find in supermarkets for this purpose. Instead use unsweetened cranberry juice or cranberry extract tablets available from health food stores.
If you are running even a low-grade fever or your UTI is causing you significant discomfort, then you should opt to see a physician for treatment.
Definitive diagnosis will be made on the basis of a urinalysis done on a clean, mid-stream catch specimen of urine. Blood, pus and/or bacteria will be present in a urinalysis that’s positive for a UTI. Occasionally a urine culture may also be ordered to test for specific strains of bacterial infection. Other tests your physician may order if he or she thinks your infection may be more serious include blood cultures and a CBC.
Treatment Options
The first line of treatment for a simple UTI is antibiotics. Commonly used antibiotics include Amoxicillin (Amoxil, Trimox), Ciprofloxacin (Cipro), and Sulfamethoxazole-trimethoprim (Bactrim). Symptoms often respond to treatment within 24 hours, but it is important to complete the antibiotic regimen even if symptoms have disappeared otherwise the implicated bacteria may develop a resistance to that antibiotic.
Your doctor may also prescribe medication called Phenazopyridine hydrochloride (Pyridium) to control the burning sensation you experience upon urination. One side effect of Pyridium is that it turns your urine bright blue!
If your UTI has made you extremely sick or you are incapacitated in some way that makes your doctor think you will be unable to adhere to the antibiotic protocol (as sometimes happens with elderly patients), your doctor may recommend hospitalization so that antibiotics and fluids can be administered intravenously


42 Comments
Hi,i am 24 year old gentleman from Ghana.I’m experiencing a frequent unation expecially during the night.I have gone 4 medical check up bt no problem was detected bt i was given some drug by the doctor and yet still the symptom exists .Pls i need help is there any herbal remedy 4 treating it(frequent urination)?Thank you.
Hi Daniel, I am Nicholas 36 yrs of age and I’ve been suffering from urine problem for about 2yrs now, I’ve done various tests and nothing came up. No prostate enlargement, no infection, clear urine test but I still urinate frequently during the day and night. I want to know the problem and how can it be treated.
Going to the Bathroom more times than nessary, I’d common among High Sugar Levels. Being a Diabetic myself, I know this problem all to well! Get tested if you are a Diabetic.
Hi Daniel,
I would strong recommend corn silk tea. Buy fresh corn and remove the silk from the corn, steep and drink.
Recipe
2 ears of corn (remove silk)
1 cup of spring water
Bring water to a boil and then remove from heat. Add the corn silk and cover the pot. Let it sit for 15 minutes. Pour the water into a cup and enjoy. Do this 2 to 3 times a day. It has amazing healing properties for the urinary tract and bladder. **You can also reuse the same silk for a couple additional servings.
Hi,
I am 26 years of age and I am suffering from frequent urination, I have to urinate after every 30-35 minutes and I drink just 5-6 glasses of water everyday.Everytime I urinate the urine volume is very less approx 50-60 ml.I underwent a couple of diagnosis but there is neither blockage,nor prostate, nor I am suffering from Diabetic and with reckons to urinary frequency as suggested by the Doctor I have taken drugs but of no success.could you please suggest any natural remedy to overcome the same.
I am 30 years old. Female. I have frequent urination every 5 mintues I get the urge and get plenty of urine. the phyisician says nothing wrong with the kideny , diabetes. They said its overactive bladder and non of the medication works. The situation is harder at night.I have been with this problem since I am 24 and its getting worse.
Very good for woman problem
Hello Diana I am a student of Natural/holistic medicine future Narupathic doctor. Sorry about your problem try Grapefruit juice 100 % natural squeezed from the fruit with 2 spoons of Rice Vinegar twice per day. Hopefully this will help you, I give you my mail if you have any questions. izzyamor@outlook.com
Hi Diana, I too have urinary incontinence. I had a bout a year ago for like a month, and now its been almost 3 months with the constant feeling of having to go and literally cant hold it. My bladder is also irritated..hurts and sometimes stings a little but I have no infection present. I am 31 and also suffer from nerve issues. So im wondering if this could be a nerve issue and how to tell. Has yours gotten any better? Does anyone have any advice? Ive started taking Magnesium..just the regular over the counter 400 mg tablets a few days ago. We will see how it goes.
My father is 80 years old. A few months ago has removed prostate. After surgery he urinates so involuntary. Analysis of the urinary bladder results in infection. All other tests come out very well. So my father’s health is very good. During surgery the doctor found that urinary bladder is thus increased,or in other words tired, according to the doctor.
Please I would like to know in these conditions is there hope for normal urination and what treatments to use against infection.
Thank you,
alma
Hi i am 28 yrs old and i am suffering from this frequent urination ant it is only on day time and i don’t have any symptoms of diabetes and a vegetarian too. pl help me with some natural medicine to come out of this.
hi, I am 62 year old male. I am having the problem of urinating sensation while walking. I am a non smoker and non alcoholic , and eat mostly eat vegetarian food eating more vegetables and fruits. during night I have to pass urine two or three times from 10 PM to 5 AM. kindly advise me the proper treatment.
I am wondering why I seem to have more frequent urinations during the day (at work) than at night. I drink mostly tea an water at the office. I drink about 1.5 lts of water in a day and had to go urinate 4 times before lunch. I drink 1 lts in the midnight at home but other then relieving myself just before bed and first thing in the morning, I never wake up in the night needing to go. Does sitting in an office chair create a faster process for the water I consume at work. I am 36 male and uncomfortable in abdomin, chest and uncomfortable in breathing? I dont have UTI and my sugar is normal. And my tongue decomes sour in the morning after urinate.
my name is jess my E mail adress is alyih20@msn.com I have a problem when i
get up to urinate at night my heart speed
up a little and pound i hsve been to ucla
had a prostate greenlight operation ABOUT eighteen month ago and had a B/O test AND DOES NOT HAVE CANCER EVERY NIGHT
WHEN I URINATE MY HEART SPEED UP ENOUGH
TO STRESS ME OUT NEVER BOTHER ME DOING THE DAY HAVE YOU HAD ANY ONE WITH THE SAME PROBLEM OR ANY SUGGESTION WHAT COULD THIS PROBLEM BE THINK YOU JESS
urination
Sometimes when the time comes that you want to urinate go to the comfort room right away, sometimes it will trigger when you will try to stop it esp when you are busy with something. This effects will arise after you did a wrong thing. This article is great! Very helpful.
hi im a 58 year old female,with frequent urination during the day, every 35 minutes as soon as i go ,i feel as tho i can go again, this started app 2 wks ago ,went to urgent care, gyn dr, and primary care, no utis clear clean urine, no sugar n urine wats the possibilities
Hi, I am male aging almost 60. I am facing acute urination problem. Specially it increases too much in the winter. Another indication which enhances is water or tea intakes. Immediately thereafter urination starts within minutes. I do not have nay diabetic disease or any other specific syptoms. Can it be a cause of gland etc. Please send me a useful advice along with proposed medicine. Thanks a lot.
I am 27 years old.I experienced frequent urination but urine is clear and I drank lots of water.I haven’t exercise enough sitting for almost 6-10 hour a day for reading. For 3-4 days, I felt pain in my lower abdomain, first on the right, later on left for a while.I also experience back pain.I would like to what it might be and I feel panic.Please do guide me and I would be very thankful.
I observed having frequents urination especially at night for about 6 to 7 times before the day break. Athough, sometime in 2009 i was daigonised as diabetic. In a while i used to take my medicine, and urination is normal. Presently, i tries natural herm like, ginger tea because i have no money to buy my medication, yet i see no improvement of my condition. Kindly advice what to do.
hi I AM 20 years old female. I have frequent feeling of urination. after passing the urine its feel that it will more passed but dosent come only 3-4 drops come and some blood also
plz kind you sugest me for a natural solution
Dear : Shilpi I am a student of holistic/natural medicine and I am studying to be e Narupahtic
Doctor. You have a illness called NOCTURIA, the best natural treatments will be the following:
Drink Grapefruit juice with 2 spoons of Rice Vinegar twice per day. The Grapefruit has super antioxidants that regulate blood/fluid flow in the system and Rice Vinegar is a powerful antiseptic
that destroys urinary tract infections. I hope this natural treatments help you.
hi i m 48 years male old i m suffering from excessive urination at nigh since 15 years especially at winters nights
at day time i remain at normal position it get worst when i take tea or eat rice at night i goes to bath room for urination about five to seven time and did not take sleep properly in summer its gets normal please suject good remedey or medecine
Hi
whenever I drink I feel like to urinate and I urinate the same amount of water out. I feel like drinking water all the time and then urination happens . I have no pain or irritation during urination and no problem at night. please advise me on this problem
hey
i am a 18 year old male suffering from urge urination. need to urinate after every 2 minutes. it makes very difficult for me to go out from home even to school. Visited doctors but they said this is due to stress but have no stresss. please help me to overcome the problem its getting worse day by day. Having this prob from last 5 years. please help me out. its a humble request
Iam 28 age . Iam suffering from urine incompleteness
After urinate after 2min some drops of urine will come again and again
Iam 28 age . Iam suffering from urine incompleteness
After urinate after 2min some drops of urine will come again and again . Pls give me reply in my email or….
hi i m 67 year old i have urine problem 30 to 35 minute ago i go to take bath in everytime when i urine i feel pain and my breath is to fast please tell me some suggestion
It’s interesting reading this article and many others none mention about candida and parasites (which roughly 85% of the american population are overun with, its an epidemic but most cant be traced through usual doctor methods and are the cause of so many serious conditions but are practically unspoke of! )I have an overactive bladder and am currently trying to cure it. My brother had a much worse bladder condition which he has just cured hallelujah! He had it since he was young and had to get up often 6 times + in the night. Hes discovered it was caused by a type of candida (a fungus) that irritated the bladder and has cured it through A raw vegan diet and the turpentine treatment just raw gum turpentine (pine tree oil) and sugar cubes! Look it up its amazing stuff our grandparents/ great grandparents used but seems to have been forgotten.
I am 25years old male, I urinate every 30min…. please, am in need of your help on this…..
hi am joel chitaya,i have a problem of frequent urination,some days am okay then some days after urination i dont feel the satsifaction,i still feel the urge to urinate but when i try to,i only produce few or no drops but the urge still doesnt go away,i want to know what the problem is and how can it be treated
i am 28 years old, i have this frequent urination problem. i don’t drink much water still i have to go so many times. also i feel a push in my bladder that i have to go every time . i had all my blood and urine test nothing came up. now my doctor ask me to go for urologist but my appointment is so far. i want some natural remedy . can you please recommend me something.
thanks
I’m 47 year woman having trouble of passing unknowingly urine. I have diabetes problem. Pl. suggest ayurvedic remedy.
Please my name is Evans(male) I am suffering from frequent urination. I urinate often and I don’t take too much water too but when I urinate, the urine come more. Also I find some sore around my organ
M 28yr old i hv urin prblm urinate after again i felk like to Pass the urin . aftet urinate some drops of urin come again n again
I am suffering From urethral stricture which Make me painful and frequent urination .l need a natural solution to the problem.
gajanan
whenever I drink I feel like to urinate and I urinate the same amount of water out. I feel like drinking water all the time and then urination happens . I have pain on lift side of bladder . please advise me on this problem
I’m 29 years old and I had suffered from cystitis for over 2 years. I had to urinate frequently during the day and night. It’s so awkward to find a toilet everywhere because of the urinary frequency and urgency. Every time I went to pee, I could feel the pain and burning. A herbal medicine called diuretic and anti-inflammatory pill helped me get rid of the infection completely. It’s really efficient.
I have these hard callouses in my left hand which refuses to leave. And my hands also turn white when dipped in water for a while. What am I suffering from
My strategy worked!
Last night , I had the same problem. I felt the urge every one minute after going to toilet . It not only disturbed my sleep but felt terrible! It seems like whole mind is focussing on the pressure of bladder. So, I opt to distract my mind my listening to a song and verbally reciting sth…i.e only meant to distract,my mind.. It worked wonder ! I had a good sleep then. Those people , who found no serious result from medical check up.. Plz, try to distract your mind and you will get good sleep . Urge of peeing went off naturally… It looks like a psychology problem at one hand . I hope this could help some people.
Hi, my name is Patricia n I am 22 years of age, I have been experiencing this for quite sometimes n its gone but now it returns n I really want to know to cure this because it disturps my sleep at night n also I am university student n I have a lot of assignments to do but when this urination thing happens frequently it slowen the process of my school work as well. Please help me
Hi, thanks for your insightful article. To the list of botanicals to strengthen the prostate and urinary system, you might also add stinging nettle, widely available and used in Europe, and also a Chinese herb commonly called “he shou wu”. Pumpkin seeds and he shou wu are both rich in zinc, which strengthens the prostate and fertility in general. Stinging nettle (Urtica doica), also commonly known as nettle, and available in the wild over vast parts of the earth, is rich in protein, calcium, iron, and carotenoids, by various accounts. I use both nettle and he shou wu. They work for me – to prevent frequent urination and to strengthen the prostate. They may or may not work for you.
I am 24 years old. I have frequent urination every 5 mintues I get the urge and get plenty of urine and as soon as i go ,i feel as i have to go again. the phyisician says nothing wrong with the kideny , diabetes and i have undergone all the possible tests but nothing found. They said its overactive bladder and non of the medication works. The situation is harder at night and many times in office too that i have to go for urination after every 10 minutes.I have been with this problem since I am 16 and its getting worse.
Kindly suggest me with any of the possible medicine or treatment.
thanks alot.
Pulkit
Mob. : +91 8439577119
+91 7057354386
E-mail : pulkit.jhajharia@gmail.com