What Are Varicose Veins
Varicose veins, also known as varicosity and varicosis, are veins that have become twisted and engorged due to the collection of an abnormal amount of blood. Varicose veins are sometimes painful and can happen to any veins but most often affect the veins of the legs and feet, which is the result of walking and standing upright, increasing pressure on the veins in your lower body.
Symptoms of Varicose Veins
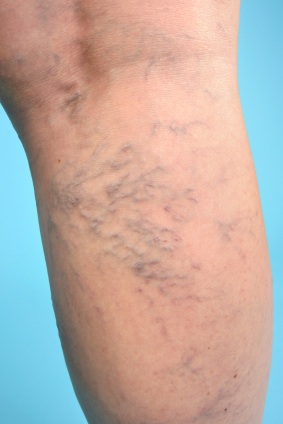
For some people, the only symptom of varicose veins is visual, as pain does not always, or even usually, accompany the condition. Signs of varicosity include veins that are a dark blue or purple color and that are visible beneath the skin. The veins will also appear to be twisted or misshapen and engorged or bulging. You may also see a mild swelling of the ankles, and possibly some skin discoloration.
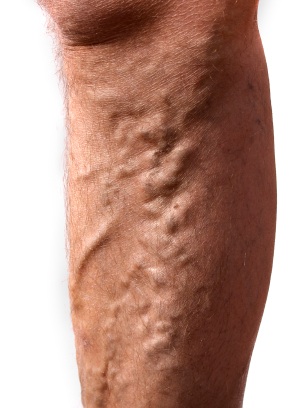
For some sufferers of varicose veins, pain will accompany their visual symptoms. There will be an aching or heavy feeling to the affected area. Swelling, muscle cramping, or a burning sensation may occur, which can be worse after a prolonged period of sitting or standing. You may also experience a persistent itch over the affected veins. In more severe cases, you may develop skin ulcers near your ankle. This is a symptom that should not be ignored and medical treatment should be sought. Varicosity symptoms tend to worsen over time, and women who are menstruating may experience heightened symptoms of their varicosity, as increased progesterone levels contribute to varicose veins.
You may be able alleviate some of your symptoms with self-care: elevating the legs, wearing compressed stockings, and exercise all work to ease painful symptoms and may prevent worsening symptoms.
Varicose Veins? Get Remedies Fast!
Causes of Varicose Veins
The purpose of your veins is to return blood to the heart, which will be recirculated throughout your body via your arteries before the process is repeated. There are valves within your veins assisting in this process. The valves open to allow the blood to flow back to your heart, and close again to stop the blood from returning. Assisting in this process are also muscle contractions to help move the flow of blood, and elasticity in the vein walls. When any of these processes cease to function correctly, varicose veins may result.
There are a few reasons normal vein functioning might cease. The valves in your veins may be congenitally weak. In other words, they may have been defective since birth. Varicose veins are thought to be a hereditary trait, so this weakness may be genetic. Age also increases the likelihood of developing varicose veins. As your body ages, your veins may lose some of their elasticity and as a result become misshapen. Age may also weaken the valves in your veins, allowing the blood that should be flowing toward the heart to back up and pool within the vein. When this happens, the vein becomes swollen and twisted. The blue appearance of the veins is due to the fact that the blood trapped in the vein is deoxygenated (oxygenated blood flows through the arteries to nourish the body, whereas veins carry back the deoxygenated blood to the heart).
The most common secondary cause of varicose veins is pregnancy. Factors contributing to pregnancy-related varicosity are numerous. First, there is an increase in the volume of blood in pregnant women, which is coupled with a decrease in blood flow between legs and pelvis. The purpose is for greater fetal support, but one side effect may be varicose veins. The second contributing factor is the extra weight a pregnant woman has in her uterus, which exerts extra pressure on her legs. Third, changes in the levels of the hormones estrogen and progesterone work to relax the vein walls, further contributing to varicosity. Typically, varicose veins that develop during pregnancy improve without medical intervention within a few months of delivery.
Risk Factors of Varicose Veins
While a definitive cause for varicose veins is unknown, experts agree that certain factors increase your risk of developing varicose veins. Age is the greatest indicator. Between the ages of 30 and 70 you stand a greater chance of experiencing varicosity. This is due to the increased wear and tear on the veins as you age, which affects blood flow. Your veins have to fight gravity to return the blood to your heart, and when they are weakened with age – both the walls of the vein and the valves blocking blood from flowing backward – it may cause the blood to back up and collect in the vein.
Sex is another indicator of increased risk of varicosity. Women are more likely than men to develop varicose veins, at nearly double the rate as men do. Hormonal changes during pregnancy, menstruation and menopause may be the contributing factor here. The female hormones (estrogen and progesterone) work to relax the vein walls which reduces their effectiveness. Genetics also play a role. If a family member has varicose veins, you are more likely to develop them as well.
Added strain to your body may also increase your risk of developing varicose veins. Obesity adds pressure to your legs and therefore your veins. Certain chronic conditions also add a strain to your veins: constipation, an enlarged prostate resulting in urinary retention, chronic coughing, and any other condition which may cause you to strain for prolonged periods of time and therefore increase the pressure on your veins. Prolonged standing also places a greater strain on the legs and may lead to varicose veins, especially if the valves have been weakened by age, pregnancy, obesity, or prior leg injuries or surgeries.
Prevention Tips
Researchers have been unable to definitely say what causes varicose veins, which makes the question of prevention tricky. In addition, there is no guarantee against developing varicose veins, however carefully you follow prevention techniques. There are a number of options, though, to prevent varicose veins, or prevent current varicosity from worsening.
Improving overall health will help prevent varicose veins, especially improving circulation and muscle tone. By exercising, maintaining a healthy weight, and eating a diet high in fiber and low in sodium, you will improve your circulation. Toning your muscles also assists in this, as muscle contractions help move the flow of blood in your veins, so keep your legs fit via walking, bicycling, or climbing stairs. Moving your legs on a regular basis will also help. If you are required to sit for long periods of time, periodically flexing your ankle and calf muscles – at least a few times every hour – will help pump the blood through your legs. To do this, simply pump your foot up and down, mimicking the walking motion, at least 10 times per leg every hour.
Another technique to prevent varicose veins is to elevate the legs, making sure your feet are in a higher position than your heart. If your job requires long periods of standing or sitting, sleep with your feet elevated, propping them with cushions to keep them elevated above heart level. You may also want to wear compression stockings, a kind of support hose that provide an outer pressure that may improve circulation and increase blood flow. Compression stockings should especially be worn during long periods of sitting, whether at work or during long plane or car rides.
There are avoidance techniques you may practice as well. Avoid prolonged periods of time standing or sitting. Also, you should avoid high heels which put undue pressure on your legs. Tight clothing or hosiery, which restricts blood flow and disrupts circulation, should also be avoided to help prevent varicose veins. You should also avoid excess heat on your legs. Heat contributes to the swelling in varicose veins, so avoid hot tubs and baths that are too hot.
Testing for Varicose Veins
The first step in diagnosing varicose veins is a physical exam. The physical exam will include your doctor looking at your legs while you are standing to check for any swelling. Your doctor may also ask for a description of your symptoms, such as any pain you may be experiencing in relation to your varicose veins. Generally speaking, varicose veins are diagnosed strictly through these visual means and there are no other tests necessary to confirm a diagnosis of varicose veins. However, your doctor may decide the need for other tests is indicated based on any complications you may experience from your varicose veins, such as blood clots.
An ultrasound is the most common test requested. This is a noninvasive procedure and is used to ensure your veins are functioning normally and there is no clotting. An ultrasound technician will usually perform this test. The technician will apply a warm gel to the area, which helps to produce a clean picture for the technician. He or she will then rub a small device called a transducer against your skin, over the gel, which sends images of your veins to a monitor so that the technician and your doctor may check for vascular health.
Treatment
Home Remedies
The greatest treatments for varicose veins are self-care such as the above described preventative measures. Topping the list are elevating your legs, exercise and diet, and compression stockings. Exercise will improve your circulation and overall health. Work with your doctor to determine the appropriate level of activity for you. Following a healthy diet not only will help you shed any extra pounds adding stress to your veins, but a low-sodium, high-fiber diet prevents water retention and constipation, both of which contribute to swelling and varicosity.
Compression stockings are your best bet for self-care, and should be tried before seeking medical treatment. These support hose apply constant, uniform pressure to your legs, improving circulation. They are worn all day and come in varying “strengths” of compression, including prescription strength, but don’t necessarily need to be tight, just strong. They can be bought at most pharmacies, but before purchasing your pair, use a tape measure to measure yourself according to the chart you’ll find on the package to ensure you buy the right size.
Compression stockings may be difficult for certain people to put on, so if you have arthritis or weak hands, there are devices available to help you put on these stockings. These self-care remedies are very effective, with little to no risk of side effects. If your varicose veins are pregnancy related the condition will typically improve within three months of delivery.
Medical Treatment Options
If self-care does not work and your varicose veins have become painful, or if the area is swollen or tender or discolored, or if a rash appears, you need to seek medical attention. There are a number of medical treatment options available to treat varicose veins. Be sure to research your choice carefully, and check with your primary doctor before having any treatments performed.
Sclerotherapy
The most common medical treatment for varicose veins. A solution is injected into the affected vein, which triggers a swelling of the vein walls, causing them to stick together and finally shut. This stops blood flow and the vein turns to scar tissue and eventually fades. The same vein may need to be injected more than once, depending on the severity of the varicosity.
This is an effective treatment when done correctly and the treatment can be performed in your doctor’s office. There are various possible side effects, including stinging, cramping, redness, skin ulcers, and bruising at the injection site. Discoloration may appear around the treated vein, though it usually disappears. The vein may also become swollen or develop bits of coagulated blood, which is not dangerous. Applied heat and aspirin should reduce swelling, antibiotics may be prescribed for any infection, and the bits of coagulated blood can be drained.
Electrodessication
This is very similar to sclerotherapy, but instead of sealing off the vein with the injected solution, an electrical current is used. Possible side effects are also very similar.
Laser Surgery
The laser projects a strong stream of light directly onto the vein, causing it to fade and disappear. This procedure is very accurate when done correctly and only damages the affected area. This noninvasive procedure does not include any needles or incisions, and the patient will only feel a slight pinch when the laser hits the patient’s skin, which can be soothed by cooling the skin. The treatment takes 15 to 20 minutes and will need to be repeated two to five times, depending on the level of varicosity the patient is experiencing. Normal activity may be resumed immediately following treatment. Side effects may include some redness or swelling to the treatment area, but these typically last only a couple of days. Also, the patient my experience some discoloration of the affected area, which should disappear after one to two weeks.
Closure
Closure involves placing a catheter into the vein, heating the tip of the catheter, and then removing the catheter. As the heated catheter moves through the vein, the vein collapses and seals itself shut. The patient’s healthy veins should then restore blood flow. This surgery is typically used on very large veins, and the only side effect is bruising.
Ligation or Stripping
This is typically an outpatient procedure (occurring in an operating room) and requires either a local or general anesthesia. It entails tying shut the affected vein and removing it through a series of small incisions. Ligation or stripping is usually performed on surface veins and removing them does not negatively effect circulation. As with any procedure, if a general anesthesia is used, the patient runs the risk of cardiac or respiratory complications. As in sclerotherapy, blood coagulation may occur, but rarely is a problem as the collected blood settles on its own. At the incision points infection, inflammation and redness may occur, and possibly permanent scars. Nerve damage is another possible side effect, as nerve branches are difficult to avoid in this surgery. A deep vein blood clot is the most serious possible side effect of this procedure, and there is a risk the clot could travel to the heart or lungs.
Ambulatory Phlebotomy
In this procedure, a special light is used to locate the varicose vein. Next, small incisions are made in the skin and surgical hooks are used to pull the vein out of the leg. This is generally an outpatient procedure that requires anesthesia to the incision area. The most common side effects are bruising and mild scarring and patients may return to normal activity the following day.
Endoscopic Vein Surgery
This surgery is used to treat more severe instances of varicosity that include skin ulcers. Anesthesia is required and the procedure is approximately one to two hours in length. A skinny camera is inserted into you leg to enable the surgeon to see your veins and then close the varicosities. Next the veins are removed through small incision in the skin. Activity must be kept to a minimum for a couple of days after surgery, and may slowly return to normal activity over the next few weeks.
Alternative Medicine
Horse chestnut seed extract is an herbal remedy that may be used to treat swelling and discomfort associated with varicose veins. It is used in Europe to treat chronic venuous insufficiency. CVI may include leg swelling or itching, varicose veins, leg pain, and skin ulcers. Side effects of horse chestnut seed extract are no different than with placebos. However, there is an increased risk of low blood sugar, so consult with your doctor before taking and use with caution if you are a diabetic.

4 Comments
I’m treating mine with aloe vera with excellent results, twice a day, every day.
Dear rocio barrientos
pl elaborate application of aloe vera in vercios vein pain.
is it external applicaion only
haridas
I am going to give the aloe vera a shot. Externally and internally. I have a very large vein I have began using Apple Cider Vinegar on today.
I read where you treated with Aloe Vera. Did you used it externally or internally and did you use the juice or gel. I have a huge varicose vein and now have phlebitis in that leg. Thank you for any help you can give me.