Burned Mouth Syndrome (BMS)
Overview
Burning tongue syndrome (BMS) has many different alternative names including scalded mouth syndrome, burning lips syndrome, glossodynia, glossopyrosis, stomatodynia, stomatopyrosis, and oral galvanism. Regardless of the name, the condition involves chronic, burning pain in the tongue, gums, lips, and inside of the mouth.
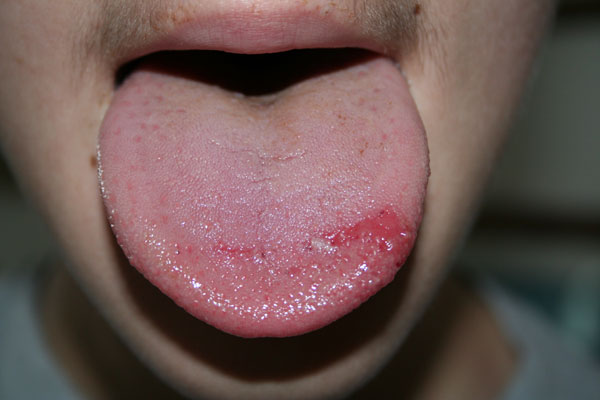
While there aren’t any visible signs or lesions to observe, the very real pain can range from moderate to severe, and some have compared its intensity to that of a toothache.
BMS usually begins without any recognizable trigger, and may last for a few weeks, months, or even years.
Diagnosis is usually a process of ruling out other possible conditions, and treatment varies from lifestyle changes in diet and behavior to the administration of traditional drugs.
Two thirds of those reporting BMS will have recovered in 6-7 years as constant pain and discomfort becomes more episodic. There is no known prevention for this problem at present.
Symptoms
The most obvious symptom of BMS is an unpleasant to painful burning sensation on the tongue, lips, gums, palate, throat, or even in the whole mouth. It is also possible to have a numbing or tingling sensation in the mouth or on the tip of the tongue.
Burning Tongue? Get Remedies Fast!
Interestingly, most patients report that they awake with little or no pain and the intensity increases as the day progresses, peaking by bedtime. They experience little or no pain during the night hours, starting the cycle anew each day. Some report having a very dry mouth and increased thirst. Another symptom may be a loss of taste or a change from normal to a bitter or metallic one that lingers in the mouth. These evidences of BMS may be continuous or periodic.
Causes
While the actual causes of BMS have yet to be been clearly established, it seems that the condition can be divided into two general categories. When the outbreak has no identifiable cause, it is treated as “primary” or “idiopathic” BMS. Researchers suspect that there is a dysfunction of the sensory and taste nerve of the peripheral and/or the central nervous systems.
The cranial nerves are also associated with the taste sensations. “Supertasters,” those people with a really high density of the small papillae that contain the taste buds seem to be slightly more prone to BMS, possibly because all those extra taste receptors are surrounded by basket-like clusters of pain neurons that may fire up if the taste buds stop functioning, as often happens during menopause.
Secondary BMS
If an underlying problem is identified and BMS becomes a symptom of the greater illness, the term “secondary” BMS is used. As mentioned previously menopause seems to be a key player in this health issue. As a woman’s estrogen levels drop in pre-menopause, it fades from her saliva as well.
With the loss of function of her bitter taste buds, it would appear that the pain neurons are activated and BMS may be the result. The fact that 40% of menopausal women suffer from this condition that starts about 3 years before menopause and lasts as long as 12 years after, seems to support this theory.
Other Possible Causes
- Oral candida (yeast infection of mouth)
- Hormonal deficiencies or abnormalities
- Diabetes (specifically Type 2)
- Dry mouth
- Blood abnormalities (anemia, dyscrasias)
- Medications (especially those given for high blood pressure)
- Endocrine disorders (hypothyroidism)
- Nutritional deficiencies (B vitamins, niacin, folic acid, iron, zinc)
- Allergies (food, gum, toothpaste, mouthwash)
- Gastric acid reflux
- Dental procedures
- Dental disease
- Unhealthy oral habits (biting tongue, thrusting tongue, grinding teeth)
- Chronic infection
- Inflammatory disorders
- Tobacco use
- Oral cancer
- Nerve damage
- Too many acidic drinks
- Mouth irritation (excessive tongue brushing)
- Use of ACE inhibitors (angiotensin-converting enzymes)
- Dentures (stressing muscles and tissues or causing allergic reaction in surrounding tissues)
Risk Factors
Most sufferers of BMS are middle-aged women between the ages of fifty and seventy years. They are seven times more likely to be affected than men, which may support the argument for hormonal imbalance experienced during menopause as the most frequent underlying condition.
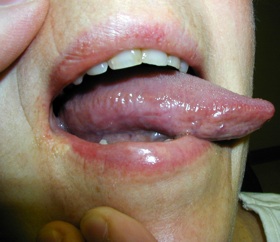
There doesn’t appear to be an identifiable trigger, and the onset is usually spontaneous. Approximately 30% of those diagnosed with BMS report recent dental procedures, illnesses, or newly prescribed medications in their history intake.
Other important factors seem to be stress or a traumatic life event, allergic reactions, upper respiratory infections, and excessive taste bud loaded papillae.
Tests and Diagnosis
Because there is no present consensus on the origins or causes of BMS, most doctors will try to diagnose this condition by process of elimination, ruling out all other possibilities. The patient can typically expect a review of personal medical history and current medications being taken. The mouth will be thoroughly examined and cultures taken.
The doctor will want to know about the symptoms being presented as well as the oral habits and mouth care of the patient. Most doctors will want to do a complete general medical examination while they search for an underlying condition that may have triggered this attack. Blood tests will be part of that process as well. It may be necessary to have an imaging test such as an MRI or CT scan.
Allergy tests and saliva measurements are often included, as is a test for gastric reflux. Finally, the last item will probably be a psychological questionnaire to analyze the levels of stress the patient may be experiencing.
Complication
While each person who suffers from BMS is unique, some associated problems seem to be held in common. It is not unusual for patients to express difficulty in sleeping. Whether this insomnia is caused by increased levels of evening pain or the stress associated with having this illness is uncertain. In a similar fashion, it is not always clear whether the accompanying depression is a cause of the BMS or a result of trying to deal with this illusive illness.
Irritability and anxiety are understandably often part of the package too. Some patients report difficulty eating because of the persistent pain in their mouths or on their tongues or lips. Others stop or decrease their times of socializing because of the discomfort and distraction that BMS causes.
Treatment
Since there is no known cure or universal treatment for primary BMS, each patient will be dealt with according to the individual presenting symptoms. The goal will be to alleviate the pain as much as possible, or if that fails, at least to manage it.
There are several drugs currently available including Klonopin, a lozenge type form of the anti-convulsant drug clonazepam. Patients have reported some relief with this medication.
Secondary BMS Treatment
Concerning secondary BMS, the treatment protocol involves identifying the underlying cause and then addressing it as a way to eliminate the presenting burning mouth or tongue issues. Recommendations can include traditional drugs, alternative health care, and lifestyle changes. It would appear that the combination of lifestyle adjustments and alternative health practices offers the best results for many patients. However, some underlying conditions require very serious attention and become the primary focus of treatment, at least initially.
Alpha-lipoic acid is a strong antioxidant that seems to benefit BMS suffers. Oral thrush medications can be prescribed as well as saliva replacement products. There are also special oral rinses and mouthwash products that a doctor may include in the treatment regimen.
Home Remedies
Some of the simplest home remedies can actually bring almost instantaneous relief to the BMS sufferer. They are as uncomplicated as sucking on ice, keeping one’s mouth moist by sipping extra water, and increasing daily intake of certain foods. Eating “plain” food and lots of boiled vegetables is a good place to start. Foods high in Vitamin B need to be included in the menu.
Meat, brown rice, fish, wheat germ, whole grain cereals, and soybeans are all great sources of Vitamin B. Also, foods rich in iron such as red meats, liver, cashews, figs, and Special K cereal are recommended additions, especially in cases where the underlying condition may be anemia. Adding certain fresh fruits and vegetables to a healthy diet can also help.
Applying glycerin to the tongue has been reported to bring relief, as has eating honey with milk. It seems the combination increases the blood flow to the tongue which encourages a healthier response from the pain neurons.
More Homeopathic Remedies
Another homeopathic treatment involves applying lavender oil to the tongue and leaving it there over night. Lavender oil is actually a powerful antiseptic. Some doctors recommend topical Capsaicin, a cream pain reliever made from chili peppers. Its purpose is to desensitize the tongue and mouth from the burning sensations.
There are simple lifestyle choices that can also make a difference in reducing the pain from BMS. Sugar-free gums will keep the mouth and tongue moist. Avoiding alcohol and tobacco are also important. Both smoking and chewing tobacco can be problematic if BMS is diagnosed.
Ironically, while the doctor may have prescribed Capsaicin cream for your tongue, it is best not indulge in spicy foods because of added irritation within the mouth. Others to avoid include acidic foods and liquids such as some fruit juices. Eliminating soft drinks and coffee are important changes to one’s diet as well.
Toothpaste
It may be necessary to switch out a favorite toothpaste, especially if the one in question contains sodium laurylsulfate. Baking soda is always a good safe alternative. While in the bathroom, check out the mouthwash also, to make sure there is no alcohol in it.
Behavior Concerns
Although hormonal imbalances have taken first place as a plausible cause of BMS, to date there is no conclusive evidence that hormone replacement therapy has had a significant effect in successfully treating this problem. If a doctor determines that psychological factors such as stress, anxiety, or depression are the causes and not the symptoms of BMS, antidepressants may be prescribed.
Cognitive behavior therapy has also been used to treat this condition. The bottom line may be to make as many lifestyle changes as possible to reduce the negative effects of stress and anxiety in one’s life.
Cost
The expense of finding relief from the pain of BMS is directly related to the number of professionals one may visit and the amount of health insurance in place. Many sufferers first consult their dentist because they view their mouth problems as dental care issues. From there, they may consult a family physician who will probably send them on to a specialist.
Add to these visits, the cost for all the preliminary tests, and the price continues to rise. Throw in a CT scan or MRI and it’s beginning to be really costly for the person without good health insurance. Some of the drug regimens are expensive, and so is a visit to the psychologist. If the patient doesn’t already suffer from anxiety or depression, rising health costs may do it.
The best approach would seem to be to try the easiest and least expensive treatment suggestions first. It may not be necessary to seek further expensive care. To the sufferers of BMS, this is no minor problem that can be easily overlooked. Imagine a toothache that lasted for years. For some, any price is worth getting relief.
Progress
In the past, because of the lack of physical symptoms in the mouth and on the tongue, many patients’ complaints were not taken seriously. Add that to the fact that the majority of complainers were middle-aged women in the throes of menopause, and the seriousness of the ailment often came into question. It was not unusual to be told that one was imagining the discomfort.
Today, however, the medical profession is more aware and sympathetic to this problem. Increased research seeks to understand the etiology and the pathogenesis so that more effective treatments can be prescribed. The dental field is also involved since dental procedures and problems seem to sometimes precede the onset of BMS.
It is to be hoped that in the near future, much more definitive knowledge will be available and better treatment protocols in place. Until then, trial and error of both traditional drug therapies and alternative health recovery plans, when combined with relevant lifestyle changes, are the best chance one has to find relief from the pain of BMS.

26 Comments
how about like hot coffee burns in the mouth
Day 1: Strange blisters started to form on the roof of my mouth. Day 2: Blisters grew larger. Later that evening, I pressed my tongue to the roof of my mouth and popped the blisters, then rinsed. Day 3-4: The roof of my mouth was still raw and sore, but the blisters did not come back. My gums on my upper right back teeth started to hurt and my teeth felt like they were going to fall out. Eating became painful (stung). Day 5-6: In addition to my gums hurting, my inner cheeks felt sore and started to burn. Took vitamin B complex, some iron, got an acupuncture treatment (to relieve the heat from my mouth). Day 7: My gums and cheeks and roof of mouth felt better, but my tongue was now raw in patches and at the tip (and burned). My lips on the inside also looked as though the skin had worn off. I chewed sugarless gum all day, rinsed a lot, continued with B vitamins and iron. Day 8: Tongue felt a bit better, gums, cheeks, and roof of mouth completely better, lips still raw. Used a lot of petroleum jelly (even on the inside) and dabbed lavender oil inside my mouth (lightly). I had read that BMS could last for several months, but I think I’ll be fully recovered in about 10 days. This is an extremely uncomfortable problem. It actually hurt to eat anything dry at all (bread, sunflower seeds, etc.). I’ve been hydrating a lot and feel a lot better. Note that I had a minor dental procedure about 3-4 days before the original BMS presented itself. I had anesthesia (local) and topical resin was applied to my front teeth to cover some missing enamel. Not sure if it related or not. No other symptoms, illnesses, or blisters or anything on the outside of my mouth or anywhere on my body.
I have had BMS for about 10 years and been to many professionals but no cure.
I put Ambesol on my gums everynight to try to sleep but it doesn’t help much and
am on 100 mg of Amitryptalene(sp).
Anyone else have success for this condition?
Hi Barb,
I recently have been suffering from BMS. To relieve the pain I use: 5ml each, 1 part Milk of Magnesium 1 part children’s liquid Benadryl and 1 part water. Mix in a small cup and swish. It stings a little but this really relieves the pain for quite a while. Good luck to you .
I am a 48 year old female, post hysterectomy leaving the fallopian tubes, and have recently started hormaone therapy and I have had tongue problems ever since. For e, it started by feeling like my tongue was too big, after that subsided the tip of my tongues has felt just like I had sipped too hot coffee! It’s been three weeks and I see my doctor in another two weeks so we shall see what happens next.
I found this site very interesting and helped immensely i have had numerous visits to the doctors had blood tests i dont think they have ever taken me serious well they will now i know i have some idea of what i am talking about as before i hadn’t a clue what it could be i’m almost positive it is BMS as i tick most of the boxes, i’m not one for looking on the internet but was so distressed with it, thanx for the good info
Long time sufferer
burning mouth syndrome;I CAN TELL YOU NOW THAT I AM 67 YEARS OLD AND HAVE HAD THIS SYNDROME SINCE 1998.IT HAS BEEN WITH ME EVERY DAY OF MY LIFE SINCE THEN. NO AWARDS HERE ONLY SKEPTICISM FROM DENTISTS AND DOCTORS OF SPECIALTIES. THEY ARE TAKING IT SERIOUSLY NOW,I JUST READ ON LINE ABOUT CLONAZEPAM,I THINK GENERIC NAME IS KLONOPIN,IWILL TRY IT,IF I CAN CONVINCE DOCTOR TO PRESCRIBE IT .GOD BLESS YOU ALL.
Hi all.. Thought I was alone with this issue until I found this site! I’m 25 and have had this burning/itchy very painful sensation on the tip and middle of my tongue. It has some fine cuts on it, and have had it for about 2 weeks.. This is the 2nd time its ever happened and soo unbareable! Doctors can’t seem to find the cause of it which makes it even harder to deal with! Sucking on an icecube relieves it for about 2 minutes.. Waiting for bloodtests to come back with some answers and hopefully treatment.
Peppermint works well in relieving symptoms , I stopped taking Amplodipine for BP and my BMS has pretty much gone away, now its just a hardly noticeable taste . like would would get from bitting into a green Persimmon
I have been suffering with this ailment for about 6 months now, seen doctors, dentist, peridontist and lastly a professor of dentistry who arranged for me to see a hypnotist. The first visit (this week) she didn’t put me under but instead tried to find out as much as possible about my life, stresses etc. It is now not so much about the pain which only occurs occasionally, but with a VENGEANCE. My problem, whch is actually driving me crazy,is that my tongue seems
to have developed a vivid imagination and
I believe I have cotton thread wound
round my teeth, which actually on
occasion hurt because it gets wound round so tightly. My tonge feels huge cavities
behind 2 teeth and this tastes so vile, as well as the latest sympton which feels
like scales or plaque round all my teeth so as you can imagine I have a toothpick
in my mouth permanantly. Anyone ever have this? Please let me know so that I know I’m not going mad!
like crazy. I also have huge cavities at the back of 2 teeth, I
like mad
I started in November 2013 with Burning Mouth Syndrome. I am 73 years old. I am desperately trying to find out if any cure or help has been found?? If anyone can help me, please send me information. I have tried so many products, but without any permanent relief!
Has any research regarding BMS been done since 2012?
I recently have been doing research for a friend on Burning Mouth Syndrome. I am involved with essential oils and using a holistic approach to treating many types of health symptoms. In my search for suggestions, I have learned that Frankincense Oil has helped someone with regard to the symptoms related to Burning Mouth Syndrome. I would not use just any Frankincense Oil, but a therapeutic grade oil, which cannot be found in retail stores the majority of the time. I have also read that Myrrh Oil is very cleansing for oral health and the throat.
A common use for Myrrh is to use it as a mouthwash to help prevent dental infections. Although the FDA has approved myrrh as a safe food additive, taking concentrated forms or high doses can have unwanted side effects. It is best to ask your doctor or a licensed healthcare provider to avoid any complications. Due to its anti-inflammatory and anti-bacterial properties, myrrh can help relieve inflammation of the mouth and gums caused by diseases such as gingivitis and mouth ulcers. It can also be used as mouth rinse to prevent gum disease. It can also freshen your breath and commonly used as an ingredient in mouthwash and toothpaste.
Due to its antiseptic properties, frankincense oil is a great addition to any oral hygiene regimen. Look for natural oral care products that contain frankincense oil, especially if you enjoy the aroma. It can help prevent dental health issues like tooth decay, bad breath, cavities, or oral infections. You can also consider making your own toothpaste by mixing frankincense oil with baking soda.
Feel free to email me anytime. I am a Wellness Advocate with the largest organization in the country today regarding therapeutic grade essential oils and how they can help address many health and wellness issues and symptoms. I hope you have found this information helpful and may God put his healing hands upon you and assist you in this challenging time.
Hello….thank you for your response on the BMS which I have had periodically for a year. It comes and goes and I can never figure out how I got rid of it. I did not use frankincense or myrrh but will try these. I LOVE essentials oils and am an ardent enthusiast for their use. I just don’t put time into it because I am overextended on current life demands. So , I am very appreciative of folks who garner wisdom as you apparently have and are generous in spirit to share it. You said email you anytime so thank you. I will keep your contact and try not to abuse your generosity. At the present moment I have people who are committed to selling me essential oil products but not so much on solutions on their use (beyond the typical lavender for calming, lemongrass for mosquitoes, etc.)
Sharon Green
Do you take Blood Pressure meds, like Amplodipine , that is a major contributer to BMS ,
My sympathies with all the suffered of BMS who have posted here. Homeopathic remedies are those that are made and prescribed in a very particular way and only by professional homeopaths. Lavender oil on the tongue may be helpful but it is NOT homeopathic.
I had no idea that this was an actual thing!I thought that I must have burned my tongue some how and it was not healing. I love spicy foods and cinnamon, but when I eat them now it is painful! I eat with a cold glass of water next to me all the time. I had some dental work before this began and never thought there was any connection. However, I am a 55 year old woman and just had carpal tunnel surgery, so there is an inflammatory component. This has been very enlightening!
Physician prescribed Fluconazole 150 for fungal infection. Just an hour after taking Flucon, started developing burning sensation of lips. By the time I woke in up the morning, lips were swollen, mouth had severe burning sensation, palms &feet severely tingling. rash at multiple places on the body.
Went to a dermatologist. He has now put me on streoid (mecapred 8 mg). Fungal infection and palms+feet tingling improving. But burning mouth and swollen lips still troubling a lot. Looking for some home remedies for burning mouth since already on too much medication.
Hi all you BMS sufferers. I can honestly say I have never been more miserable than I have the last 3 weeks. I used a toothpaste called oral b pro expert, started to get gum shedding, really disgusting. Next thing I know I have burning gums and lips have stopped using the culprit that caused it, but the damage has been done. Can’t use any toothpaste at all, just bicarbonate and salt, what has helped though is coconut oil, I have been rinsing my mouth out with a big spoonful, takes some getting use to, but it does bring relief for a while. Am having blood tests and allergy test. Am going through the menopause so doc is checking every avenue. Am praying I will get rid of it. It’s lousy, and very depressing.
Firstly, disappointed that the site says “more homeopathic remedies” in the information section. Whoever wrote this does not know what homeopathy even is, as there are no homeopathic remedies listed. I believe you mean natural remedies. I have seen about 50 cases of burning mouth syndrome in my 35 years as a Doctor of Oriental Medicine/Acupuncturist.
In Traditional Chinese Medicine burning mouth syndrome is an imbalance/ deficiency of what is called yin- the body’s calm, cool,anti-inflammatory, quiet side. In western medicine this inflammatory condition is poorly treated. The best remedies are those herbal or nutritional supplements that build yin/reduce inflammation. Look up the Chinese herbal combinations: lui wei di huang wan(six flavor rehmannia tea pill) and Zhi bai di huang wan(eight flavor rehmannia tea pills). These formulas balance hormones and reduce inflammation. In terms of western medicine I have found alpha lipoid acid helpful. Also consider Coptis (related chemically to goldenseal) as it is antibacterial and antiviral. HSV-1 can be a contributor to this syndrome and coptis reduces inflammation and also inactivates some viruses and kills bacteria. One of my favorite remedies is Lemon Balm tea. It is antiviral, anti-inflammatory, and soothing to the nervous system.
Best way to find dr of oriental medicine that treats burning tongue. I live in northeast Philadelphia ,pa. Does acupuntor work for this. I also have sibo.
Hi Dr. Chatfield,
I have been doing some research for a friend with regard to how to incorporate Essential Oils into a routine that could be helpful with the painful sensations associated with Burning Mouth Syndrome. I have read that both Frankincense and Myrrh Oils can prove to be helpful. Possibly making toothpaste by using 1 drop of each oil with baking soda, or using as a mouth rinse as well. Do you have any opinions on this? Thank You for your input.
Does acupunture work for burning tongue
I’ve been suffering from BMS on and off for several years! I’m in my last 50’s…they have been reducing my ERT over the past year. I’ve noticed it has gotten worst since then. When a virus; such as a cold, I notice it starts up again… etc. Ice does help for a minute! Maybe my ERT needs to be increased again to see if it helps the symptoms. And I am under a tremendous amount of STRESS this past year; my Therapy dog and best friend passed away, a few months ago my Mother passed away; and I’m in the middle of a major and final move in my life. I also suffer from a Chronic Illness-Cryoglobulenemia type 2. And Living with a Cherokee Indian Hubby isn’t easy either, especially when I am from Long Island NY(originally)! Thanks for listening. I will give up my coffee; what about decaf tea, coffee, or Green tea?
Hello and greeetings!
I am a member of a 2 groups on FB…Burning Mouth Syndrome and New Burning Mouth Syndrome ! It is very interesting to join, since the science has improoved great….and there is a hope on a horyzont…..Recently also they are saying that in some cases BMS is dru to Neurothropic viruses….and many other condtions! Please come and join these two groups…people are ever so nice an you will find a lot of informatio….God bless you all-with love Zdravka Rostočil……I am also the sufferer of BMS!
Hello, I suffer BMS for more than a year, on and off. I’m 38. Managing my stress, anxeity and doing lots of meditation, relaxation helps a lot for me. Keep calm.
Hi I’m 37 & I’ve been suffering from BMS for 2+ years. I’m a recovery addict so meditation is not even a solution for me. Has anyone tried free Aloe Vera? And AHA ( Omega supplements) I’ve been trying omega 3 but haven’t seen any results. I know the symptoms worsen when stressful, so yoga (any calm environment helps)
Thanks for letting me know I’m not alone