Cracked Heels
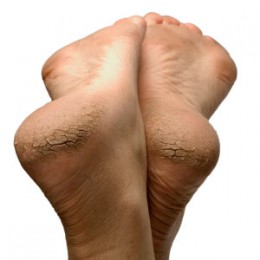
Dry skin is a primary culprit of cracked heels. The body produces no oil in the palms of hands and on the bottom of the feet.
Therefore, the area remains dry most of the time. The feet require more care than other parts of the body in order to remain moisturized and free of cracks.
Today, most individuals engage in pedicures to remove dead skin and promote healthy skin. Regular cleaning and removal of the skin through various techniques will minimize the effects of cracked heels.
Individuals who do not use proper hygiene on their feet accumulate up to 30 times more skin in that area than on other parts of the body.
Cracked Heels? Get Remedies Fast!
Heels are also more prone to cracking with age. Cracks or deep wounds may facilitate the development of infections. Calluses are thickened skin that may also form on the toes.
Where to Expect Foot Cracks
Though cracks in the skin may arise anywhere on the body, the most common is area is the rim of the heel and web of toes. This also happens to be the most frequently or constantly used part of the body. Dry skin and psoriasis are common causes of cracked heels.
Most foot problems arise due to neglect and oversight with regard to foot care. Cracked feet, corns and other common feet ailments are treatable and easily avoidable.
Avoid Infections
Cracked heels are not a harmful in anyway except when the fissures or cracks are deep. Over time, the cracks tend to become painful, and the skin begins to bleed.
This could lead to infection. This situation is avoidable. However, those already suffering from chronic ailments, such as diabetes or a low immune system, may experience more problems than people who have general good health.
Athlete’s Foot is also a common cause culprit of cracked heels.
There are several types of Athlete’s Foot that may contribute to cracked heels
- Toe Web Infection
- Moccasin Web Infection
- Vesicular Web Infection
Each of these common infections will be explained thoroughly in the causes section of this article.
Not only will attention to the feet reduce the chances of contracting Athlete’s Foot and other awful skin conditions, foot care may also release stress and remove toxins from the body.
Sufferers from arthritis, fatique and hyperglycemia may benefit from foot care, as well. Foot care will also enhance the person’s beauty. Most individuals become self conscious when attempting to wear sandals with cracked heels.
By maintaining proper moisture on the feet, individuals will feel confident about wearing sandals that expose the feet. Cracked heels will draw unwanted attention to feet and detract from an individual’s overall appearance. Podiatrists recommend focusing on the foot care each day or once per week to maintain a healthy appearance.
Alternative Names
Cracked heels are medically referred to as heel fissures. The wounds are linear and superficial in most instances. This becomes a problem when the cuts are deep into the dermis and become painful. Cracked heels may also indicate a zinc or omega-3 fatty acid deficiency.
Cracked heels may also occur due to Athlete’s Foot. Athlete’s Foot is often referred to as “tinea pedis.” This term describes an infection of the skin that may crack, scale, flake or itch. The infection is fungal and may also be referred to as the ringworm of the foot.
The fungus is in the Trichophyton family. Most individuals contract the fungus through the feet, but the disease may spread to other areas of the body. The fungus may also spread to the groin area. The fungus thrives in moist and damp areas.
Therefore, it is most often contracted in areas, such as showers or bathhouses, where people walk around barefoot. The best way to prevent Athlete’s Foot is through good hygiene. Pharmaceuticals and other treatments are available to cure the fungus once contracted.
Symptoms
Individuals suffering from cracked feet will notice small tiny lines in the feet. This marks the beginning of dry, cracked heels. In the case of Athlete’s Foot,
the symptoms may be any of the following
- Cracking
- Scaling
- Flaking
- Itching
- Splitting Skin
- Blisters
Individuals experiencing these symptoms should seek a physician or treat with an antibiotic. Several over the counter creams are available.
Other symptoms may be specific to the type of Athlete’s Foot contracted.
Some of the related symptoms to Athlete’s Foot are listed below
Toe Web Infection
When an individual contracts a toe web infection, then the skin will often turn moist or pale white. The feet may itch, burn, and develop an odor. As the condition worsens, the skin between the toes will crack, peel and become scaly.
If the condition gets even worse, a bacterial infection may also develop which may cause the skin to break down further. The skin may also blister or form a vesicular infection. The condition may spread to the lower leg. Most toe web infections will respond well to treatment.
Moccasin Web Infection
This type of infection begins with dryness, itching, burning, scaly skin, or minor irritation. Over time, the condition causes the skin to thicken and the heels to crack.
In some instances, toe nails may fall off after they become infected. Before the nail falls off, the nail will thicken and crumble. If the infection is persistent, it may often return if not treated. Good personal hygiene will prevent the disease from returning. Most of these infections are chronic and may be difficult to treat.
Vesicular Web Infection
These infections begin with an outbreak of blisters. The feet may suffer from inflammation and become red in appearance. Blisters may erupt again after the initial infection. Bacterial infections may develop if the condition is left untreated. This type of condition frequently develops when a toe web infection is left untreated. Blisters may also appear on the palms and fingers. These types of infections do respond well to treatment.
If the condition spreads to other parts of the body, the disease is no longer referred to as tinea pedis. The fungus will be called astinea corporis, which afflicts the body. Alternatively, if the fungus spreads to the groin area, it is referred to as, tinea cruris or “jock itch” or “dhobi itch.” Onychomycosis is the name of the fungus if it spreads to the toe nails.
Causes
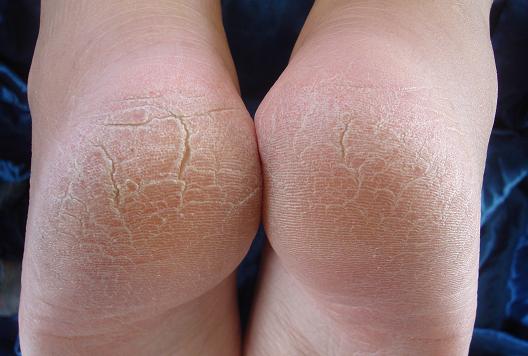
Some individuals suffer dry, cracked heels due to poor hygiene. The person may not exfoliate daily or moisturize well enough.
Additionally, it could occur because the person is not drinking enough water. Each of these factors may contribute to dry, cracked heels.
Individuals are recommended to moisturize the feet with a heavy cream and scrub daily. Petroleum jelly or other moisture rich products designed specifically for the heels may help.
Cracked heels may also indicate a deficiency in zinc and omega-3 fatty acids.
Athlete’s Foot may be contracted from moist, damp areas, such as a bath house or shower. It may also be contracted by sharing towels or shoes with someone who has Athlete’s Foot. Tinea pedis develops in a variety of ways. The fungus may also be treated in a variety of ways. To determine the cause and treatment, identify the type of Athlete’s Foot the individual is experiencing.
Some of the most common types of Athlete’s Foot are listed below
- Toe Web Infection
- Moccasin Web Infection
- Vesicular Web Infection
Other causes include
- Psoriasis
- Eczema
- Thyroid Disease
- Diabetes
- Age
- Shoes that do not fit properly
- Climate-related dry skin
- Vitamin deficiency, such as minerals or zinc
- Standing for excessive periods of time
- Heels that drag or hang over the side of sandals
Risk Factors
In general, cracked heels do not pose any risk factors as long as an fungal infection has not developed. Untreated cracked or dry heels may lead to a variety of problems.
Some of these problems may include the following
- Development of a chronic fungal disease that is difficult to treat
- Deep wounds may develop and bleed
- Fungus may spread to undesirable places on the body, such as groin area and the lower extremities
- Infection may set into the open wounds
- May be an indicator for a low immune system
- Infections such as diabetes may increase the risk for cracked heels
- Walking barefoot, sharing towels, and showering in public places with no protection on the feet may increase the risk for contracting the fungus
Seniors and people who stand on their feet frequently are most at risk for cracked heels. The condition may affect both the heels or one heel depending upon the origin of the stressor. Those who frequently shower in public places or walk barefoot are at risk for Athlete’s Foot.
Prevention Tips
Athlete’s Foot is spread from person to person. Thus, the disease is considered communicable. Since the disease is caused by the parasitic fungus, Trichophyton, individuals should take extra precautions to avoid the disease. Because the disease is a fungus it can spread easily from the feet to other areas of the body. Good hygiene is always the first step of prevention.
To avoid contracting Athlete’s Foot or developing dry, cracked heels, individuals must take the following precautions
- Avoid walking barefoot in public areas
- Avoid taking showers in public areas without proper foot protection, such as shower shoes or flip flops
- Do not share towels with other individuals
- Do not share shoes with other individuals
- Moisturize the feet with a heavy cream daily
- Remove dead skin with an abrasive, such as a pumice stone, foot scrub, or loofah
- If you contract a fungal disease, use the medication or antibiotic for the prescribed period of time
- If the fungus is not cured after the medication, seek the help of a physician
- Wear shower shoes
To prevent fungal spread in the home, individuals should take the following precautions
- Spray the tub and bathrooms with disinfectants each use to avoid the spread of the fungus.
- Launder towels, sheets, socks, underwear and bed clothes in hot water to kill the fungus.
- Change towels and bedsheets at least once per week
- Do not share towels with other household members
- Use a separate towel when drying areas that are infected
- Wash feet between toes with soap and water
- Dry feet thoroughly after showering
- Treat feet and shoes with over the counter drugs
Other prevention tips
- Limit the amount of sweat on the feet
- Wear well ventilated shoes
- Keep feet dry
- Wear lightweight cotton socks to reduce sweat, moisture wicking polyester socks with anti-microbial properties are the best
- Wash socks in hot water
- Wear a different pair of shoes everyday to keep feet dry
- Replace sole inserts in sneakers frequently
- Replace old sneakers and exercise shoes
- Wash with a soap that contains an antimicrobial and antifungal agent
- Regularly soak feet in vinegar and water
- Change socks frequently
- Use foot powders and antiperspirants
In general, people who have a genetic predisposition to dry, cracked feet should exfoliate regularly to remove dead skin and calluses. Use creams with alpha or beta hydroxy acids. Alternatively, urea also helps to remove dead skin. Creams with dimethicone penetrate the epidermis. This provides a protective layer to the skin which seals in the moisture.
Smelly feet often accompany dry, cracked feet. Smelly feet are not attractive. There are over 250,000 sweat glands in each foot that contribute to sweat and smelly feet. According to physician, Issac Tabari, smell is caused by “bacterial decomposition of excessive perspiration.” Companies have developed sprays and foot pads to combat sweating and odor.
Some of the popular drugs that assist with this common problem are as follows
- Dimethicone : Decreases moisture, sweat and therefore, fights Athlete’s Foot
- Triclosan: Eliminates odor causing bacteria through an antibacterial agent
- Chlorhexidine digluconate: Eliminates odor causing germs through an antibacterial agent
- Grillocin: Neutralizes foot odor
- Menthol: Masks odor through a cooling agent
Test and Diagnosis considerations
Athlete’s Foot can be diagnosed by a physician, dermatologist, pharmacist, or general practitioner. During diagnosis, the physician will physically inspect the skin to determine the cause of the cracked, dry skin. If the physician suspects the condition may be eczema or psoriasis, the physician may inspect the skin under a microscope with a potassium hydroxide mixture.
This test is often referred to as the KOH test. The physician will scrape the affected areas of the skin and inspect them under the microscope. The test usually yields an excellent positive predictive value. A biopsy may also be taken in order to evaluate for histological examination.
Treatment Options
Herbal and Home Remedies
- Apply cracked creams on your heels and drink a plethora of water.
- Eat foods rich in Vitamin E: Cereals, green vegetables, nuts, wheat germ, and nuts
- Eat food with Calcium and Iron: Yogurt, ice cream, meat, chicken and fish
- Eat foods rich in Zinc: Oysters, chicken, kidney beans, yogurt, crab
- Eat food rich in Omega-3 fatty acids: Fish, flaxseed oils
Tea tree oil may provide relief from itching. This is primarily due to its relation in the histamine response.
However, the treatment of Athlete’s Foot with tea tree oil has not been proven to entirely relieve symptoms. Further studies are being conducted to determine the evidence conclusively.
Onion extract has been proven to be effective in conditions against the Trichophyton fungus. A 3 percent solution is the recommended concentration of the onion extract. Ajoene is a compound found in garlic. The popular compound is often used to treat Athlete’s Foot. Boric acid is often applied in socks to prevent Athlete’s Foot. The treatment is effective for recurring infections.
Additional Treatment Options
Putting baking soda on the feet or sprinkling baking soda in the shoes changes the pH and alleviates symptoms associated with dry, cracked heels. Baking soda also eliminates odor. Epson salts will also soothe the feet if several tablespoons are applied to warm water. The salt will also loosen the dead skin and aid in the removal of dead skin.
Ionic foot spa is purported to remove toxins from the body. This is accomplished through electrolysis that removes toxins from the body by opening pores. The toxins are released into the water. Apply a banana to the dry or cracked area of the heel. Leave the substance on for 10 minutes and rinse. Soak feet in lemon juice weekly for 10 minutes until the feet are smooth.
Each day soak the feet in warm and soapy water. Then apply Vaseline and the juice of a lemon. Allow the mixture to absorb overnight while wearing socks. Apply glycerin and rose water daily.
Pharmaceutical
Severe fungal infections may require that individuals take oral anti-fungal medication in order to alleviate or cure the symptoms. The most common ingredients in prescription anti-fungal drugs include ketaconazole, itraconazole, naftifine, and nystatin.
Topical ointments may come in the form of a spray, powder, cream or gel. Most of the over-the-counter drugs contain miconazole nitrate in a 2 percent concentration and tolnaftate in a 1 percent concentration. Terbinafine is also a common over-the-counter drug. Zinc oxide based diaper rash ointment may also alleviate the symptoms. Talcum powder may also absorb moisture to fight infection.
Those who desire a topical treatment should not simply select an anti-itch ointment. These ointments may promote moisture and exacerbate the condition. Experts recommend the use of gels instead of creams for application of topical treatments. Lamisil and naftin both are available in a gel that penetrates the skin more rapidly than creams.

4 Comments
I had dry cracked heels, for that i have taken some warm water and added salt, lime water or 1 tsp of turmeric powder in to it. I put my foot for 15 mins then rubbed with hard stone finally applied crack cream it works for me.
I AM DIABETIC WITH THOSE CRACKES ON THE HEEL MY PODIATRIST HAS PRECRIBED TRIAMCINOLONE ACETONIDE CREAM 0.5 % IT DOES NOT SEEM TO BE WORKING. ANY SUGGESTIONS PERHAPS ANOTHER MEDICATION THAT DOES WORK FOR THIS CONDITION?
I purchased an over the counter foot cream called “CeraVe Renewing SA Foot Cream”. It is sold at Wal-Mart, K-Mart and major pharmacies. I had cracked heels for years and despite using oils, creams and many other types of treatment, nothing worked.
I used this CeraVe Renewing SA Foot Cream for 2 weeks and I no longer have any cracks in my heels. It has softened the skin on my feet, improved their color and is even improving my toenails. The SA in this cream stands for Salicylic Acid, which helps exfoilate the skin. My callouses are completely gone and needed no pumice stone or other filing down of the callouses. This cream alone, worn at night with socks on, and a light coat on my feet in the day has completely resolved my condition.
Hello there, Kim, I have taken some warm water and included salt, lime water or 1 tsp of turmeric powder into it. I put my foot for 30 minutes at that point rubbed with hard stone at last connected break cream it works for me. In any case, as of late I confronted a similar issue. Would you be able to please recommend me for the long-term solution?