Diabetes Mellitus: Management and Remedies
Diabetes mellitus is the inability or compromised ability for the body to produce or assimilate insulin. Insulin is a hormone produced by beta cells in the pancreas and released into the bloodstream to help regulate serum glucose (blood sugar) levels. Insulin helps to transport glucose to cells, where it is either converted to energy for use or stored as glycogen, or fat. Inadequate assimilation of insulin prevents the body from efficiently converting glucose to energy. The inability to convert glucose to energy results in high blood sugar levels (hyperglycemia), which manifest with various symptoms collectively known as diabetes. According to the American Diabetes Association, 23.6 million people in the United States have diabetes (2007 data).
When glucose cannot be transported to the cells, excess glucose remains in the bloodstream. The body has several mechanisms to get rid of this excess. Water is excreted by the kidneys so that the glucose is diluted and eliminated through urine. Thus, people who have diabetes may experience thirst and frequent urination. Urine may also have a “sweet” smell. If glucose is not available for use as energy, the body then begins to use fat cells to produce energy, which can have serious side effects.
Types of Diabetes
Several types of diabetes have been identified, including prediabetes, type 1, type 2 and gestational.
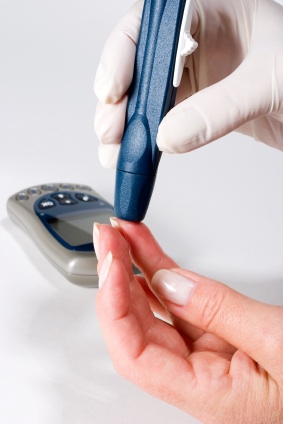
Prediabetes is a condition which may lead to diabetes. People diagnosed with prediabetes can often prevent the onset of diabetes by establishing healthy eating habits and exercising. Symptoms may be subtle or non-existent. The condition is identified in consultation with the physician who will perform a series of tests and examinations. People who are overweight have a higher risk of becoming diabetic.
Type 1 Diabetes
In type 1 diabetes, previously known as juvenile-onset or insulin-dependent diabetes, the pancreas is unable to produce insulin. In this type of diabetes, the body’s immune system attacks and destroys the beta cells in the pancreas, resulting in the inability to produce insulin. Scientists do not yet know why this occurs, but it is not caused by overeating, poor diet or other controllable variables. Type 1 diabetes is relatively uncommon and often develops at an early age, or before the age of 30, although it can occur at any age.
Type 2 Diabetes
Type 2 diabetes, also known as adult-onset or non-insulin-dependent diabetes, is the condition in which the body does not produce enough insulin or cannot effectively utilize the insulin produced. In some instances, insulin is produced but is not utilized by the cells of the body; this condition is termed “insulin resistant” or IR.
Diabetes Mellitus? Get Remedies Fast!
Type 2 diabetes is more prevalent in certain population groups including Native Americans, Hispanics, African Americans, Asian Americans and Pacific Islanders, although it occurs in all population groups. Once considered to be a disease that manifested later in life, it is now becoming prevalent at alarming rates in younger adults and children. Type 2 diabetes can often be prevented and controlled by diet and exercise. Obese people are more likely to develop type 2 diabetes.
Gestational diabetes is the occurrence of raised blood glucose levels in the mother during pregnancy, usually after the 20th week, when the mother has not previously been diagnosed as having diabetes. After delivery, the condition often resolves by itself, but some women with gestational diabetes will develop type 2 diabetes later in life.
Symptoms of Diabetes
The symptoms of type 1 and type 2 diabetes are similar but may vary in intensity. Symptoms of type 1 diabetes may occur quickly, whereas symptoms of type 2 diabetes may be more gradual and less intense. People with type 2 diabetes may be undiagnosed for years because the symptoms are mild or occur gradually and are not noticed.
The most common symptoms of diabetes include:
- Increased thirst
- Increased urination
- Fatigue
- Blurred vision
- Sudden weight loss
- Constant hunger
Additional symptoms may include:
- Drowsiness
- Nausea
- Tingling or numbness in hands and feet
- Cuts and bruises that are slow to heal
- Frequent infections or recurring infections that are slow to heal
The release of energy from fat cells produces ketones, which make the blood too acidic. This can lead to diabetic ketoacidosis, more prevalent in untreated type 1 diabetes. Symptoms of ketoacidosis include:
- Abdominal pain
- Nausea
- Vomiting
- Excessive thirst
- Rapid breathing
- Breath has “chemical” smell like nail polish
Diagnosis
To diagnose diabetes, a fasting blood test is done, normally after eight hours or overnight without food. Fasting blood levels should fall below100 mg/dl (milligrams per deciliter). Two occurrences of fasting blood sugar levels higher than 126 mg/dl indicate diabetes. Blood testing after food can also be used to determine glucose levels. Glucose levels over 200mg/dl indicate diabetes. Based on these tests, the doctor will discuss treatment options with the patient, taking into account the type of diabetes, stage of the disease, lifestyle, age and diet.
Complications and Risk Factors of Diabetes
Many serious health conditions can occur as a result of diabetes. Risk factors increase over time and are higher with poor management of the disease. High levels of glucose in the blood over time result in narrowing of blood vessels and build-up of fatty acids in large blood vessels. This, in turn, affects circulation. The most common complications include neuropathy, atherosclerosis, heart attack and stroke. Other complications include kidney failure, muscle deterioration, poor circulation, increased infection, resistance to healing and blindness.
Diabetic neuropathy is present in the majority of patients with diabetes. Numbness, tingling and pain in hands and feet are common; because blood flow is reduced, nerve damage results. This can affect the ability to feel injuries or for wounds to heal, resulting in chronic or recurring infections and even gangrene. In severe cases in which gangrene is present, amputations may sometimes be required.
Nerve damage can also affect the stomach and intestines, resulting in nausea, ineffective intestinal contractions or slow emptying of food from the intestines.
Diabietes and Heart Disease
More serious is the relationship between diabetes and heart disease. Heart disease is the leading cause of death among diabetics. High blood pressure, heart attack and stroke occur at higher rates among diabetics. Because of the damage to nerves and poor nerve receptivity, chest pain and other symptoms associated with a heart attack may not be felt by a diabetic patient.
Treatment
Proper diet and exercise are critical elements in the control and treatment of all types of diabetes.
In type 1 diabetes, insulin must be used to regulate blood glucose levels. Insulin must be used for life. Several types of insulin are available, classified by the length of time it takes to reach the bloodstream and the amount of time it remains in the bloodstream. Selection of the type of insulin to be used is made in consultation with the doctor and dietician. Lifestyle, age, commitment to management of the disease and diet are considered in the decision about which type of insulin to use.
Careful monitoring of insulin levels is important. A drop in insulin levels can result in hypoglycemia, or low blood sugar. Symptoms include disorientation, weakness, headache, trembling or unconsciousness. This condition requires immediate intervention by administering oral glucose such as fruit juice, sugar water, candy or honey if the person is conscious. If the person is unconscious, glucagon should be injected.
In type 2 diabetes, several options are available for patients, including medicine, diet and exercise. Diet is perhaps the most effective and the most manageable remedy in the control of type 2 diabetes. Recent research has substantiated the importance of a diet high in complex carbohydrates, high in fiber, low in fats and moderate in protein. The goal in management of diabetes with diet is to regulate the amount of insulin that enters the bloodstream. Thus, consuming small meals throughout the day, eating at regular times and carefully selecting foods can have a dramatic effect in the positive management of diabetes. Avoiding foods that cause insulin levels to rise or spike is important.
Glycemic Index
The glycemic index is often used to identify foods that are high in carbohydrates, which may exacerbate surges in blood sugar levels and insulin production. The glycemic index measures how much blood sugar is raised after eating a food. Low glycemic index foods are slow to be digested and absorbed, causing a low rise in blood sugar. Although the glycemic index has application to diabetics, the amount of dietary fiber in the diet is equally important. Often foods high in fiber have a low glycemic indexl. Foods with high levels of dietary fiber cause a slow rise in blood glucose levels and help to keep insulin production stable. Examples of foods with high fiber and a low glycemic index include:
- Whole grains
- Oats
- Lentils and other beans such as chick peas or black beans
- Spaghetti
- Some fruits such as apples, cherries and grapefruit
Exercise has been proven to ameliorate the complications and intensity of diabetes. Because the complications of diabetes affect many systems of the body, exercise is a main factor in leading a healthy, longer life as a diabetic. Exercise lowers blood pressure, lowers bad cholesterol levels and lowers the risk of stroke and heart disease. It also lowers blood glucose levels, helps to keep the circulation system healthy and contributes to weight loss. Exercise also helps to reduce stress. It provides muscular fitness, which helps to avoid falls and provides overall strength.
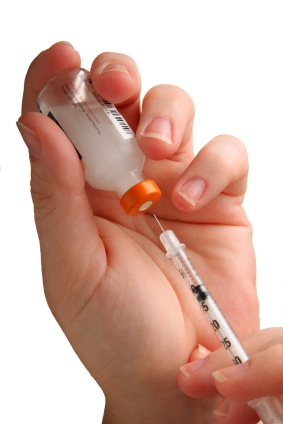
Medications may be prescribed to help control type 2 diabetes. Several types of oral medications are available: those that stimulate production of insulin in the pancreas, those that lower blood sugar and those that slow digestion of starches. One of these types, or a combination, may be suggested by the attending physician. If type 2 diabetes eventually results in lack of insulin production, the patient must then also use insulin.
Alternative Treatments
Alternative treatments for diabetes have been used in other cultures around the world for centuries. Allopathic medical research is now exploring many of the medicines, herbs and treatment methods used in these other systems. Often, as new potential treatments are identified, these discoveries are lauded by the media as wonder cures. Over time, as research progresses, scientific evidence provides a more balanced view.
Ayurveda
Ayurveda, meaning science of life, originated in India and is practiced in many countries in Asia and around the world. Ayurveda uses herbs and other natural substances to treat many health conditions including diabetes.
Ayruveda is a system of medicine with treatment given by a trained vaidyan, or Ayurvedic doctor. Medicines are carefully chosen for the specific condition to be treated. Many vaidyans prepare their own medicines, or work in treatment centers that prepare medicines. These remedies are usually in the form of tonics, oils, powders and pastes which combine specific ingredients in carefully measured amounts to produce a formulated concoction prescribed for specific symptoms.
Rather than focusing on a named disease or syndrome such as diabetes, the vaidyan takes into account the entire medical condition of the patient. Age, specific symptoms, diet, stage of the disease, body structure and lifestyle are among the factors considered. Patients may be asked to severely modify their diets, such as avoiding all fat or not eating any acidic foods, while under treatment.
Treatments Under Scrutiny
Some of the herbs used in Ayurveda are under study by Western medical practitioners and are advocated by consumers who want natural treatments. The temptation to select a “natural herb” as a treatment for diabetes should be done with caution because the herb used in isolation, or the part of the herb used, may not provide the desired results. For example, the herb Ficus racemosa is used to treat several conditions including diabetes; however, the latex sap is used for diarrhea, the leaves are used for bilious excesses and the root is used for diabetes. Combinations of different herbs also produce different results; particular combinations may promote weight loss, open blood vessels or lower cholesterol levels.
Herbal Remedies
The National Institutes of Health’s National Center for Complementary and Alternative Medicine provides discussion of specific herbal remedies for diabetes. The summaries include results of studies and clinical trials, side-effects and proven efficacies. Some herbal therapies have shown promise in lowering blood sugar levels or stimulating production of insulin in the pancreas; people on insulin using these remedies are advised to closely monitor insulin levels to avoid hypoglycemia.
Some herbal remedies that may be effective in controlling diabetes and the complications resulting from the disease are as follows.
Coccinia Indica
Coccinia indica, kovakkai, is a small cucumber-like vegetable consumed in India. Some studies show promising effects in its ability to lower blood glucose levels. A study in rats combining this vegetable with Abroma augusta suggested that the combination has a greater effect that either one by itself in lowering glucose levels.
Curcuma Longa
Curcuma longa, turmeric, is used to treat many ailments. It has known anti-inflammatory properties, and has been shown to improve circulation and reduce cholesterol. Turmeric is used for treatment of diabetes in India. Clinical trials in animals show promising results for glycemic control. Its other effects are of benefit to diabetics as well. .
Gymnema Sylvestre
Gymnema sylvestre, cluster fig, is a tree native to southern India. Encouraging research suggests this herb may reduce blood sugar levels. It is also suggested that it may block sugar receptors on the tongue, thereby reducing appetite and sugar cravings.
Momordica Charantia
Momordica charantia, bitter gourd, is a vegetable used in India in the treatment of diabetes. The vegetable is diced and boiled in water, which is consumed as a broth. Scientific studies evaluating its effectiveness in reducing blood sugar levels are inconclusive.
Trigonella Foenum-Graecum
Trigonella foenum-graecum, fenugreek, is traditionally used in India in the treatment of diabetes. The seeds are roasted and ground, added to water and consumed one hour before food each morning. The fiber-rich seeds slow the absorption of glucose, which aids in lowering blood glucose levels and regulating insulin production.
The use of herbs as a part of the treatment regimen for control of type 2 diabetes is promising. Western medical scientists are evaluating these potential treatments through controlled studies and clinical trials.
Costs of Diabetes Treatment
The primary costs of diabetes treatment can be relatively low if the disease is well-managed and the patient does not develop complications. Proper diet and exercise are key factors in achieving health and lessening the risks of complications. Poorly managed diabetes can lead to other serious health problems. The costs associated with the complications of diabetes can be high.
For people with type 1 diabetes, daily insulin injections are required. Regular medical check-ups are advised to ensure that other health problems do not go unchecked. The costs of insulin, needles or insulin pumps and glucose monitors and strips are basic to proper care for type 1 diabetes.
People with type 2 diabetes may have costs for oral medications, glucose monitors and strips and routine doctor’s visits. Costs for prescription medications vary; calling pharmacies to determine prices can help to keep costs down. If more than one type of oral diabetes medication is required, the combination may be available as a single pill rather than two, which can help to reduce costs.
Avoiding Treatments
Skipping doses in order to save money is not cost-effective. Unchecked high blood glucose levels will require more medication in the long run and the risk of developing other complications of diabetes increases.
Because heart disease is more prevalent in diabetics, additional medication for cardiovascular management may be required. Kidney failure is another serious complication prevalent in diabetics, often resulting in hospitalization and dialysis.
Although the costs of medications may appear to be high, not taking them, or not making regular visits to the doctor can result in serious health problems that may require hospitalization and days away from work. Actively managing diabetes by adhering to a proper diet, taking medications as directed and exercising is the best way to reduce overall costs and maintain health.

No Comments