What is Psoriasis?
Psoriasis, also called plaque psoriasis, is an unpleasant dermatological condition that affects about 2% of the population, roughly six million people. It is characterized by red, scaly and itchy skin. Depending on the severity and stage of the rash, it can also appear silvery, shiny and flaky. Psoriasis is not a medical emergency; rather it is a chronic disorder that has periods of increased flare-ups as well as calming periods. The exact cause of Psoriasis is unknown.
Some researchers believe that it is a disorder of the immune system, while others think it is more of an allergic reaction to ambient stimulants. Gene mutation has also been suggested as a possible cause of Psoriasis. There are variants of the disease and the names reflect the differences. For example, when there are distinct teardrop-shaped red marks it is called “guttate psoriasis”, (guttate is Latin for “drop”). Other types of psoriasis include pustular psoriasis in which postules are also present with the rash; inverse psoriasis, where the rash affects areas where skin touches skin such as under breasts, in folds of genitals and armpits; and erythrodermic psoriasis, where there is pronounced reddening and the rash is more widespread.
Where Does it Occur?
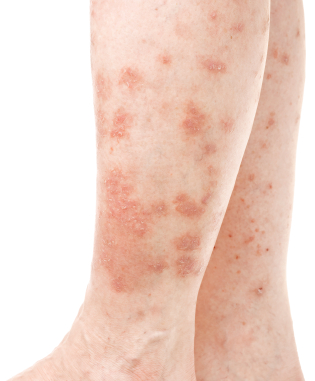
Psoriasis break-outs occur most often on the areas of the body where there is movement. That is, where there are flexor muscles, such as the elbow, knees, arms and legs. It spreads along the outer part of the limbs, such as the shins and outer-arm. Other common sites are the scalp, palms and plantar aspect of the foot. However, it can occur just about anywhere on the body including the face, back and stomach.
This disease does not just affect the skin. It can also be present in fingernails, toenails, genitalia and inside the mouth. When it occurs in these more tender areas, it is uncomfortable and more difficult to treat. Also, in about one million psoriasis sufferers, the joints become inflamed as well. When this happens it is known as psoriasis arthritis.
What are the Symptoms of Psoriasis?
Psoriasis can be difficult to diagnoses and treat because it can be quite complicated. The patient could have one or more types of psoriasis at the same time and/or at different times in her life. Since there is more than one type of psoriasis, there are differing symptoms according to which type of psoriasis is affecting the patient. But the general characteristic that is present in virtually every variety of psoriasis is an inflamed rash, a silvery appearance and scaly, itchy patches. The rash has a distinct edging so that the healthy skin and the affected skin are side by side and there is an obvious distinction. Also, all types of the disease heal from the inside out. The affected area is quite unsightly and sufferers are understandably self-conscience when the outbreak is in an area of the body that is not covered by clothing.
Psoriasis? Get Remedies Fast!
What Causes Psoriasis?
The causes of psoriasis are not known but most in the medical and scientific community agree that there is a connection to a gene mutation. It is generally thought to be an autoimmune disease where there is a problem with the immune system caused by a white blood cell called a “T” cell. These cells are charged with defending the body against infection and viruses. However, in psoriasis, the “T” cell misfires, and instead of protecting against a foreign agent, it turns on normal, healthy cells by multiplying much faster than it should. This causes the hallmark inflammation. In about a third of the patients there is a familial history of the disease. This strengthens the argument for a mutant gene.
Psoriasis is not always acute, however. There are periods of calming until such time as an episode triggers a flare-up. The triggers are not always obvious, and include stress, infections, certain types of prescription medications, changes in climate, sunburn, injury to the area and even a specific nutritional deficiency- low levels of calcium.
What are Some of the Risk Factors for Psoriasis?
Since psoriasis is thought to be mostly hereditary, there is not much one can do in order to avoid psoriasis. However, patients almost always report their first outbreak to be after a streptococcal infection, great periods of stress, or in the presence of certain prescription medications. Smokers and people dealing with obesity are also more at risk for psoriasis, as are people afflicted with Human Immunodeficiency Virus (HIV).
There is very little one can do to avoid psoriasis if it is part of the body’s chemical makeup. But keeping the skin well hydrated, avoiding stress, smoking, obesity and heavy alcohol consumption seems to help control psoriasis outbreaks. As with just about everything else, getting enough rest, eating a healthful diet that is rich in calcium, and controlling the amount of sunlight one is exposed to all seem to be good ways to avoid psoriasis as much as possible.
Are there Diagnostic Tests for Psoriasis?
Psoriasis is usually diagnosed in the doctor’s office because of its distinct appearance. Upon hearing the patients’ chief complaint and examining the affected area, the general physician or dermatologist is able to make a diagnosis of psoriasis. In some cases, a dermatologist will take a small skin sample to study under a microscope. If this is called for, it can usually be done in the office employing a small amount of local anesthesia.
A doctor may elect to do this to rule out some of the other diseases that can look very much like psoriasis. These diseases include seborrheic dermatitis, (the most common cause of dandruff), lichen planus, ringworm (tinea corporis), and pityriasis rosea, a common skin condition that looks very much like psoriasis. Therefore, in order to be absolutely sure that the disease is indeed psoriasis, a biopsy may be necessary since all of these diseases call for different treatment plans. In place of an actual biopsy, the doctor may also take a small scraping. At this time there are no simple blood tests or other diagnostic tool to make a psoriasis diagnosis. It is important to note that psoriasis, unlike some of the other skin disorders, is not contagious.
How is Psoriasis Treated?
Psoriasis is a lifelong challenge for those who are afflicted, as there is no cure. So, treatment for psoriasis is necessarily long-term and depends greatly on the patient, doctor and their individual philosophies. Though self-diagnoses of psoriasis at home is never recommended, once a definite diagnosis is made, the patient is welcome to try home remedies. Many patients swear by herbal and homeopathic remedies to keep their psoriasis in check.
Home, Herbal and Homeopathic Remedies
The Aloe Vera plant, a succulent that is comprised of a gel-like substance inside its leaves, is pressed into service to remedy everything from a severe sunburn to a minor bug bite. To use it, one slices the leaf open exposing the watery jelly inside. Using ones’ index finger to scrape out the jelly, the patient will then gently apply the gel to the affected area.
If using the actual plant is not an option, there are creams, gels, lotions and sprays that contain Aloe vera and are quite effective in calming the redness, heat and itching of psoriasis. Aloe vera would need to be applied several times a day for a month or more before improvement begins to show. It is not a potion that leads to instant gratification.
It may seem counterproductive, but capsaicin cream is also used. Where the Aloe vera cools and calms the rash, capsaicin, extracted from chili peppers, has been known to ease the itching and reduce the inflammation of psoriasis. It is important to wash the residue off the hands after applying as it can cause discomfort and pain if it comes in contact with the eye or mucus membrane.
Fish Oil
Fish oil, the kind that is available in capsules, is also a favorite home remedy. The Omega-3 fatty acids have anti-inflammatory properties. This is taken orally, and very little, about 3 grams a day, is needed to get the desired effect.
Bath Treatments
Bath treatments and the application of moisturizers have been known to have a soothing effect. Available also are over-the-counter bath additives, or they can be made at home with Epson salts and oatmeal. Some patients swear by a mixture of wheat germ oil and castor oil in equal parts applied to the affected area. A tea made with marigold blossoms is also employed by some who want to use only an herbal, non-medicinal remedy.
Topical remedies can be difficult to maintain, especially if the affected area is widespread. It takes time to apply topical remedies such as the ones mentioned above, and in most cases the application must take place several times a day. So some patients may elect to try drugs to treat their disease.
Pharmaceutical Intervention
There are oral and injectable medications that are used to keep psoriasis in check. When electing this type of systemic treatment, the patient must be carefully followed to insure that there are no adverse effects because some of the drugs can be quite toxic. Blood tests and liver function tests are routinely done at intervals during the treatment so that the physician can insure that all is well. Women of child-bearing age are cautioned to avoid pregnancy as these drugs are not recommended during pregnancy. If a woman becomes pregnant while being treated, the treatment will stop immediately and the pregnancy carefully followed.
Some of the drugs that are incorporated into psoriasis therapy include methotrexate and cyclosporines, which are immunosuppressant drugs, and retinoids, which contain a synthetic form of Vitamin A. Corticosteroids are also sometimes prescribed. Drugs which are used for other diseases have sometimes been found to be effective for psoriasis treatment. Certain types of cancer drugs, drugs that treat leukemia, Crohn’s disease and ulcerative colitis are all useful in some psoriasis cases. There are even drugs that are prescribed after an organ transplant to avoid organ rejection that have been found to treat psoriasis as well. This is not as unusual as it seems, however, since the drug is being used as an immunosuppressant in both cases. Antihistamines, while not a cure, can and do relieve the itching caused by psoriasis.
Side Effects
As with every drug, there are always side effects to be considered and the patient must weigh the risks and benefits. Psoriasis is an uncomfortable, distressing disease that adversely affects a patient’s quality of life. Many psoriasis patients also suffer from clinical depression secondary to a lower self-esteem and extreme self-consciousness due to the unsightly nature of the illness. This can lead to social isolation, which only exacerbates an already stressful situation.
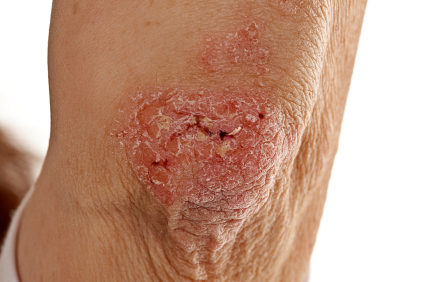
Other serious complications include bacterial skin infections resultant from repeated and aggressive scratching in attempt to gain relief from the itching. Skin infections can become quite serious and will have to be treated with antibiotics.
Another complication of untreated or undertreated psoriasis is an electrolyte imbalance in the presence of serious pustular psoriasis.
Psoriatric arthritis can be excruciating and debilitating and can lead to erosion of the joints. So when weighing the risks, benefits and costs associated with these treatments, the patient should take into consideration his quality of life, the affect his psoriasis is having on other parts of his life such as his family and his job, and whether or not the disease is relatively quiet and slow to flare up, or aggressive and intrusive.
There are studies underway to determine if phototherapy, or the application of light, is useful in the treatment of psoriasis. In countries such as Croatia, Ireland, Turkey and Serbia, doctors are treating psoriasis with a cure that involves tiny fish, called “Doctor Fish” that live in outdoor ponds but are employed to eat away at the dead psoriatic skin when it appears on feet or hands. These tiny fish gnaw away at the dead skin, leaving healthy, untouched skin beneath it. The treatment usually takes place in a spa setting, and must be repeated every few months.
Climate Change
Finally, there is the geographic cure. Some patients have found that a change in climate has eliminated or drastically cut down on instances of outbreaks of psoriasis. Areas around the Dead Sea and where the climate is sunny, hot and humid seem to be relatively psoriasis free zones, giving the impression that psoriasis may have been eliminated for those who have the luxury to move far away from their home, their stressors and their lifestyle.

6 Comments
IS PSORIASIS RELATED TO HIV?
Answer: no!
We have also found that using coconut oil mixed with lotion helps.
Not sure if I had dermatitis or psoriasis but I had a red, flaky patch next to my ear. It was smaller than a dime. Read the reviews on DermalMD Psoriasis Treatment serum and gave it a try.I would only apply it at niight. Problem solved in less than 2 weeks. It is completely gone! Excellent product.
Hello,
I hope you’re doing well. I wanted to let you know about a couple programs Healthline launched this year to support the psoriasis and psoriatic arthritis community. I wanted to spread the word about these great programs, so I thought I would share them with you.
-First, our #pselfie program is a collection of photos from people living with psoriasis. Users can upload a photo on Instragram or Twitter with the hashtag #pselfie or upload a photo directly onto our page. You can view the photos here: healthline.com/health/psoriasis/selfie/photos-and-quotes For every photo we receive, we will donate $10 to the National Psoriasis Foundation.
-Next, we have launched You’ve Got This, a collection of videos submitted by those living with psoriasis giving hope and encouragement to others with the condition. Again, for every video we receive we’ll donate $10 to the National Psoriasis Foundation. You can view the videos here: healthline.com/health/psoriasis/youve-got-this
-Lastly, we have this great visual of ‘Words You Should Know’ for psoriasis and psoriatic arthritis. All of the terms and definitions were submitted by users from our Facebook community for psoriasis sufferers. You can check it out here: healthline.com/health/psoriatic-arthritis/words-you-should-know
I’d love if you can share one or all of these with your social networks or include them as resources on your site. We’d also love if you wanted to participate in the You’ve Got This or #pselfie program. Please let me know if you can help spread the word about these programs.
Thanks so much,
Nicole Lascurain • Assistant Marketing Manager
Healthline • The Power of Intelligent Health
660 Third Street, San Francisco, CA 94107
healthline.com | @Healthline | @HealthlineCorp
About Us: corp.healthline.com
Apricot Kernel oil works wonders, and it works fast. Apply it topically two or three times a day( morning, noon, and night). It only takes a few days to notice a huge difference. It’s not expensive. Clean the area first with THEYERS Alcohol-free toner.
I love dermalmd treatment serum. Put on the effected area and feels very smooth, not sticky. Easy to absorb, feel cool and do stop itchiness immediately.