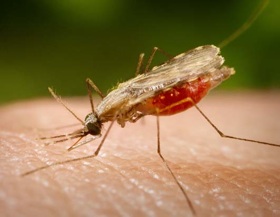
Malaria
Malaria’s widely known fear factor makes it hard to believe that this often fatal disease is caused by the bite of a tiny mosquito. While the disease in name doesn’t spark as much panic as it used to, malaria still kills more people each year than AIDS, one million of which are children.
Malaria is particularly widespread in Western Africa, although it is also a threat in regions where sub tropical conditions (and therefore, mosquitoes) exist, such as parts of Asia, Central America, and South America. Less than 1,100 cases were reported last year in the United States.
Malaria is often associated with poverty-like conditions, but this can result in a catch-22 cycle wherein the disease itself inhibits economic growth, causing poverty. Most of the cases of malaria reported within the United States stem from travelers who have visited regions where malaria is much more prevalent, unknowingly bringing the disease with them when they return.
For this reason, prevention and preventative treatment with antimalarial drugs is strongly encouraged for travelers visiting regions high in cases of malaria. In Africa, malaria is estimated to cause 20% of infant deaths, or one child every 45 seconds. Cures & remedies for malaria are constantly being developed and tested to attempt to eradicate the disease.
Symptoms
Since the symptoms of malaria can at first mimic those of septic shock and other illnesses, caution must be taken to seek the advice of a medical practitioner as quickly as possible if symptoms develop.
Malaria? Get Remedies Fast!
Malaria can take anywhere from a week to several months (and some case studies even reveal the disease taking years) to develop and spread in the bloodstream.
Generally, symptoms will develop between ten and fifteen days of contracting malaria.
Flu like symptoms, such as a fever and headache, nausea, and sweating can sometimes make the disease difficult to diagnose without a blood test.
Shivering, joint pain, vomiting, and convulsions will also show themselves individually or combined into a cycle if the patient is infected. Malaria is notorious for the vicious cycle of hot/cold that its victims endure. Often, several hours of chills and shivering are followed by hours of sweating, convulsion, and fever as the disease advances. Brain damage and anemia are known to occur in widespread form as the disease multiples within the bloodstream.
The cyclical nature of malarial symptoms makes the disease painful and unpleasant for those who contract it. Prevention and early detection are crucial with malaria, so if infection is suspected, it is important the patient address concerns with a medical provider as quickly as possible. Early detection with malaria can mean the difference between a short regimen drug treatment and a potentially fatal diagnosis.
Dehydration, kidney failure, and liver failure are some of several complications that may develop as a result of malarial infection. Untreated, when malaria isn’t fatal, it can lead to cerebral failure and
Causes
Malaria is caused by a single cell parasite which enters the bloodstream and multiplies, transmitted from the bite of an infected mosquito. Once a mosquito has bitten a person with malaria, it ingests gametocytes, a form of the parasite that will eventually mutate into malaria. The disease grows inside the mosquito, where it eventually mixes with the saliva of the insect when it bites again.
Once a human being is bitten by an infected mosquito, parasitic malaria has found a way into the body and will begin to attack its host from the inside out. The parasites develop in the liver and multiply, then rupture, eventually infecting the bloodstream. Once the bloodstream is infected, the parasites continue the progression of the disease by multiplying further and rupturing. Malaria can exist largely undetected by the body’s immune system due to its location within the red blood cells, making prevention and early detection even more crucial.
Parasite
P. falciparium, a parasite in the plasmodium genus, causes 80% of all cases of malaria and is considered the most common strain of infection. Nine in ten deaths due to malaria infection are also attributable to the P. falciparium parasite. All strains of malaria, according to research, stem from the parasitic genus Plasmodium, which has over 200 identified species.
However, only four strains of plasmodium cause malaria in humans: P. falciparum, p. vivax,p. malariae, and p. ovale. Those strains which are not in the p. falciparium species are considered easier to treat, and have a much lower rate of death.
Risk Factors
An increased risk factor for malaria contraction includes areas with a high population of mosquitoes and known cases of malaria, contaminated food, and contaminated water. If you’re going to be travelling to a remote location where the threat of malaria exists, be sure to check with your doctor on the best forms of prevention.
Other risk factors include your age, prevalence of malaria in the region in which you live or are traveling, and if you are pregnant. Typically, pregnant women are more likely than non pregnant women to contract malaria. The elderly and children are also more susceptible.
Suppressed Immune Systems
This is due to the suppressed immune system that occurs during pregnancy, as well as the relative weakness of the immune system in older people and children. Pregnant mothers, if infected, can transmit the disease to their unborn child via the bloodstream. Infants are particularly susceptible to contracting malaria.
Recently, more studies have been done examining the close relationship between infection of HIV/AIDS and malaria. People who have contracted HIV are extremely vulnerable to contracting malaria due to the weakened condition of their immune system. AIDS and malaria cause 4 million deaths a year combined; in countries where conditions are ripe for malaria, public health groups are also finding large populations of HIV infected adults, compounding both issues in terms of diagnosis, and especially treatment.
Prevention Tips
Some areas where malaria is prevalent have said to spark sort of an immunity to the disease amongst the local population, but the best prevention of malaria seems to be to attempt to eliminate or reduce the mosquito population in affected areas as much as possible. Nets, insecticide, and other control methods have a tangible impact on the number of cases when implemented consistently.
Prevention of mosquito bites to avoid initial infection cannot be underestimated in importance. Some of the most fatal strains of malaria are very resistant to conventional treatment, so the best attitude towards malaria should be the adage “an ounce of prevention is worth a pound of cure”.
A more intense method to restrict malaria outbreaks was employed successfully in the United States and southern Europe, known as vector control. Vector control uses insecticide over large areas of land to eradicate mosquito populations. The World Health Organization features several in depth research studies on the benefits of vector control for controlling malaria outbreaks. The pesticide used for this method can cause other environmental and health problems, which has led to a more recent method of attempting to develop genetically modified mosquitoes which are malaria resistant.
Prophylactics
Prophylactic drugs are sometimes used on a daily or weekly basis for preventative reasons (and occasionally as a form of treatment). Doxycycline is occasionally used as well, but the strain of malaria must be taken into consideration when prescribing preventative treatments, as resistant strains of the bacteria are known to exist.
In a recent study by the Boston University School of Public Health, vitamin A & zinc provided increased resistance to malaria, which researchers suspect is due to the known immune system boosting properties of vitamin A and zinc. This is, however, an experimental method and should not be used as the sole means of prevention.
If traveling to a country where there is a high instance of malaria, contact the Center for Disease Control (CDC) and/or the World Health Organization (WHO) for prevention tips. Some guidelines include limiting outdoor activity at night in areas where risk of infection exists, as well as contacting your healthcare provider to create a consistent regimen of prevention drugs to take before, during, and after your trip.
In this case, the most valuable prevention tactic would be to follow a strict regimen of preventative medications combined with avoidance tactics described above. Although a vaccine for malaria is not currently available, it is in development and researchers are optimistic for success in the near future.
Testing and Diagnosis Considerations

Typically, malarial symptoms are diagnosed using blood tests visually examined under a microscope, although sometimes saliva and urine are used as less invasive methods of diagnosis using optical microscopy.
The blood samples are placed on film and examined under a microscope to detect the presence of the parasite. Two samples, taken at different time intervals (typically between six and twelve hours apart) are used as checks and balances against one another to ensure the subject is being properly diagnosed.
Thin films typically allow for the best preparation technique and detection of the parasite’s appearance.
If optic microscopy is not readily available, which happens frequently in rural areas where malaria is prominent, an antigen test, or rapid diagnostic test, will be performed by technicians skilled in detection. Some of the recently available commercial tests for malaria require only a single drop of blood.
Treatment Options
Cures & remedies for malaria are constantly being developed. Hospitalization is usually required for patients with active strains of malaria to adequately provide treatment, although some less severe strains can be treated with outpatient therapy if caught early. Antiviral medications are the most commonly prescribed tools of modern medicine to combat malaria.
Industrially produced treatments include chloroquine, at one time the most popular form of malarial drug used for treatment; amodiaquine (which can be used alone or in conjunction with chloroquine); pyrimethamine, which is useful for strains resistant to chloroquine or for milder, uncomplicated cases; sulphadoxine, which is popular for treatment in clinical cases. Artemesinin, a Chinese herb, has become popular for use along with several derivatives which have had success.
A recently developed malarial drug is halofantrine, which was developed in the 1960’s at the Walter Reed Army Institute of Research. Many treatments are given at hourly intervals over a period of time set by the hospital providers. Doxycycline is another widely used malarial treatment.
Combination Therapy
Combination therapy is the most widely used form of treatment for malaria. Several single-drug treatments have been introduced to the market, but research and clinical results have proven multiple drug malarial treatments to typically be the most effective. As the most aggressive strains of malaria have grown more and more resistant to conventional treatments and techniques, new combinations and dosages are constantly being modified and introduced to implement a cure for patients.
Several treatments, amodiaquine in particular, can cause severe side effects and should be used only if the benefits of treatment outweigh the side effects. Homeopathy is gaining popularity in malaria treatment as the cost of treatment and drug-resistant parasites remain a growing concern. Goldenseal, grapefruit extract, and local herbs are often more readily available than expensive manufactured drug treatments. Quinine remains one of the oldest forms of treatment for malaria, and is still widely used in some regions of the world.
Cost of Prevention and Treatment
For preventative purposes, a rough estimate is approximately $75 US Dollars per week of malaria prevention tablets or pills. Doxycyclin is often cheaper, but many people avoid them due to the severity of side effects outweighing the initial cost savings. For people with adequate health insurance, the costs may be substantially lower.
While actual cost to treat malaria varies greatly by location, degree of infection, and strain, the overall costs are astronomical. Cost is a particular concern with outbreaks of malaria, as many areas in which the disease spreads are poverty ridden. Summarily, the disease affects those who can least afford to treat it. Treatment drugs are expensive and not always readily available. It is estimated that the average treatment for malaria in moderate cases can cost the average W. African ten days or more of full time pay.
The cost of malaria treatment in Africa is estimated to be over $800 million US dollars annually. Countries with high levels of transmission ha ve reported that approximately 1.3% or more of their annual Gross Domestic Product (GDP) is used for malaria treatment, according to the World Health Organization.

No Comments